What Are the Reasons for Denied Claims and How to Prevent Them

Denied insurance claims rarely come down to a single error. They build quietly from small, repeatable breakdowns across documentation, coding accuracy, eligibility checks, and payer-specific rules. Left unaddressed, these failures compound, slowing reimbursement, inflating A/R days, and forcing revenue cycle teams into an endless cycle of rework and appeals.
The cost of inaction is accelerating. In 2022 alone, the cost associated with denied claims increased by 67%, signaling a systemic breakdown in how claims are prepared and validated. Beyond delayed payment, denials drain operational capacity, pulling experienced coders and billing teams away from throughput and into correction mode.
For revenue cycle leaders, billing managers, and compliance officers overseeing thousands of claims each month, understanding the reasons for denied claims is a financial and regulatory imperative. As payer scrutiny intensifies and margins tighten, denial prevention directly influences cash flow stability, audit readiness, and operational control.
So what are the reasons for denied claims, and which of these risks can be identified and prevented before submission? Let’s break them down.
Quick Summary
- Denied claims follow clear patterns, driven by eligibility errors, documentation gaps, coding mismatches, and payer rule violations.
- Most denial risk appears before submission, during intake, documentation, authorization, and coding, not during adjudication.
- Preventing denials upstream is more effective than appeals, reducing rework, A/R days, and compliance exposure.
- Manual controls cannot scale as claim volume and payer complexity increase.
- AI-driven automation enables consistent denial prevention, improving first-pass acceptance and reimbursement predictability.
Table of Contents
- Why Insurance Claim Denials Continue to Impact Revenue Cycles
- Claim Rejection vs. Claim Denial: What’s the Difference?
- Top 10 Reasons Insurance Claims Are Denied (And How to Prevent Them)
- How Workflow Gaps and Payer Rules Lead to Claim Denials
- How Automation Helps Prevent Claim Denials Before Submission
- How RapidClaims Improves Insurance Claim Reimbursement
- Conclusion
- FAQs
Why Insurance Claim Denials Continue to Impact Revenue Cycles
Claim denials affect far more than reimbursement timelines. They introduce operational friction, financial uncertainty, and compliance exposure that compound across the revenue cycle.
a) Operational Impact: Denied claims force teams into repetitive tasks. Coders re-review charts, billing staff investigate remittance codes and resubmission rules, and compliance teams validate that corrections meet payer documentation standards. Each added touchpoint increases cost without improving outcomes.
b) Financial Impact: Denied claims extend days in accounts receivable and weaken revenue forecasting. Even when claims are eventually paid, delayed reimbursement strains working capital and disrupts financial planning.
c) Compliance Impact: Repeated denials signal systemic issues. Patterns tied to documentation gaps, inconsistent coding, or missed payer requirements can trigger audits, particularly in Medicare and Medicare Advantage programs where oversight is strict.
As patient complexity increases and payer rules evolve, manual denial prevention does not scale. Yet most denials are not random; they stem from known, repeatable issues that can be identified before claims are submitted.
Before breaking down those causes, it’s important to clarify terminology. Not every unpaid claim is a denial, and confusing rejections with denials often leads teams to apply the wrong fix at the wrong stage.
Also Read: A Comprehensive Guide on Medical Coding: Here is What You Need to Know
Claim Rejection vs. Claim Denial: What’s the Difference?
Knowing the difference between a claim rejection and a claim denial is important for prioritizing the right corrective action and avoiding unnecessary delays.
- Claim Rejection
A claim rejection occurs before payer adjudication. The claim is returned due to technical or data-related issues such as missing required fields, incorrect patient or provider information, invalid codes, or formatting errors. Because the payer has not processed the claim, rejections can typically be corrected and resubmitted quickly.
- Claim Denial
A claim denial occurs after the payer has reviewed and processed the claim. The payer determines the claim is not payable due to coverage limitations, missing or incorrect authorization, coding inconsistencies, or insufficient documentation to support medical necessity. Denials usually require deeper investigation, additional documentation, and a formal appeal process.
While denial codes vary by payer, the underlying causes tend to fall into a predictable set of categories across healthcare organizations.
Top 10 Reasons Insurance Claims Are Denied (And How to Prevent Them)
In most cases, denials stem from process gaps across intake, documentation, coding, authorization, and submission, not rare edge cases.
1. Missing or Incorrect Patient and Claim Data
Accurate patient demographics and claim data are essential for clean claim submission. Errors in names, dates of birth, member IDs, or policy numbers often lead to immediate rejections or downstream denials.
These issues typically originate at registration and persist through billing if not corrected early. Even small mismatches between intake records and payer enrollment data can prevent claims from being processed.
How to prevent it:
- Verify demographics and insurance details at every encounter
- Standardize data capture during intake
- Validate claim fields for completeness before submission
2. Insurance Coverage and Eligibility Issues
Claims are frequently denied when services fall outside active coverage or when eligibility has lapsed at the time of service. Common contributors include plan exclusions, expired coverage, unmet benefit limits, or unverified secondary insurance.
Coverage-related denials are especially costly because many cannot be appealed once care is delivered.
How to prevent it:
- Confirm eligibility and benefits before services are rendered
- Review coverage limitations and payer-specific rules in advance
- Keep insurance records up to date
3. Prior Authorization and Referral Failures
Many payers require prior authorization or referrals for imaging, procedures, diagnostics, and specialist visits. Claims submitted without documented approval are often denied automatically.
Authorization rules vary by payer and change frequently, making manual tracking unreliable, especially in high-volume environments.
How to prevent it:
- Identify authorization and referral requirements before scheduling
- Obtain and document approvals in advance
- Centralize authorization tracking and link approvals to claims
4. Coding Inaccuracies and Code Mismatches
Coding errors remain a major source of denials. These include mismatched ICD-10 and CPT or HCPCS codes, incorrect or missing modifiers, outdated code sets, and insufficient specificity.
When codes do not align with documentation, payers flag claims for denial or additional review.
How to prevent it:
- Provide ongoing coder education
- Conduct routine coding audits
- Validate codes against documentation prior to submission
5. Insufficient Documentation to Support Medical Necessity
Payers require clear documentation to justify billed services. Claims are denied when clinical notes do not adequately support the diagnosis, treatment rationale, or level of service.
These denials often surface after submission, making appeals time-consuming and uncertain.
How to prevent it:
- Clearly link diagnosis, symptoms, and treatment decisions
- Align documentation with payer medical policies
- Use structured templates to prompt required details
6. Timely Filing Violations
Each payer enforces strict deadlines for claim submission, typically between 90 and 365 days from the date of service. Claims submitted outside these windows are denied automatically.
Timely filing denials often result from internal delays, documentation backlogs, or limited visibility into claim aging.
How to prevent it:
- Track payer-specific filing deadlines
- Monitor claim aging regularly
- Use alerts to flag claims approaching limits
7. Duplicate Claims, Bundling, and Frequency Errors
Denials also occur due to duplicate submissions, unbundled services, or exceeded frequency limits. These issues often arise when claim status is unclear or when workflows run in parallel.
National Correct Coding Initiative edits and payer-specific bundling rules further increase complexity.
How to prevent it:
- Maintain clear visibility into claim status
- Define resubmission protocols
- Apply rule-based claim scrubbing before submission
8. Provider Enrollment and Credentialing Gaps
Claims cannot be reimbursed if the rendering provider is not properly enrolled or if credentialing information has expired. These gaps can halt reimbursement entirely.
Because credentialing updates are infrequent, issues are often discovered only after denials occur.
How to prevent it:
- Centralize credentialing and enrollment records
- Track renewals proactively
- Verify enrollment status before submission
9. Coordination of Benefits Errors
When patients have multiple insurance plans, claims must be submitted in the correct order. Errors in identifying primary and secondary coverage frequently lead to denials or payment delays.
These issues commonly originate during registration when secondary coverage is missed or outdated.
How to prevent it:
- Verify coordination of benefits at intake
- Update records when coverage changes
- Confirm payer order prior to submission
10. Billing, Place of Service, and Technical Submission Errors
Billing inaccuracies, incorrect place of service codes, and technical submission errors can also trigger denials. Common examples include misclassified inpatient versus outpatient services, telehealth coding errors, or missing required data elements.
As payer automation increases, even minor technical issues can result in rapid denials.
How to prevent it:
- Validate charges and service details before submission
- Review the place of service coding against the current payer rules
- Apply quality control checks across billing workflows
Individually, these issues may appear isolated. In practice, they point to a broader problem: workflows and payer requirements are not fully aligned. Addressing denials consistently requires upstream controls that detect and resolve risk before claims reach the payer.
Also Read: Common Medical Billing and Coding Errors and How to Protect Your Practice
How Workflow Gaps and Payer Rules Lead to Claim Denials
Most claim denials are not isolated mistakes. They are the result of disconnected workflows combined with increasingly complex payer requirements.
In many organizations, registration, documentation, coding, and billing operate as separate functions. Errors introduced during intake or clinical documentation often go unnoticed until after a claim is submitted. At that stage, teams are forced into rework, chart reviews, code corrections, documentation updates, and appeals, adding cost without improving outcomes.
Payer variability intensifies this problem. Coverage policies, authorization rules, bundling logic, and documentation standards differ by payer, plan, and service type. Static rule sets and generic claim scrubbing tools cannot keep pace, leaving organizations exposed to payer-specific denial patterns they only discover after rejection.
The issue is structural. Preventing denials requires clinical accuracy and payer alignment to happen upstream, before claims reach the payer. In most cases, the risk signals already exist; they are simply detected too late.

How to Identify Denial Risk Before Claims Are Submitted
Effective denial prevention depends on identifying risk early, while corrections are still efficient and low-cost. Most denial drivers surface during intake, documentation, coding, and authorization, not during adjudication.
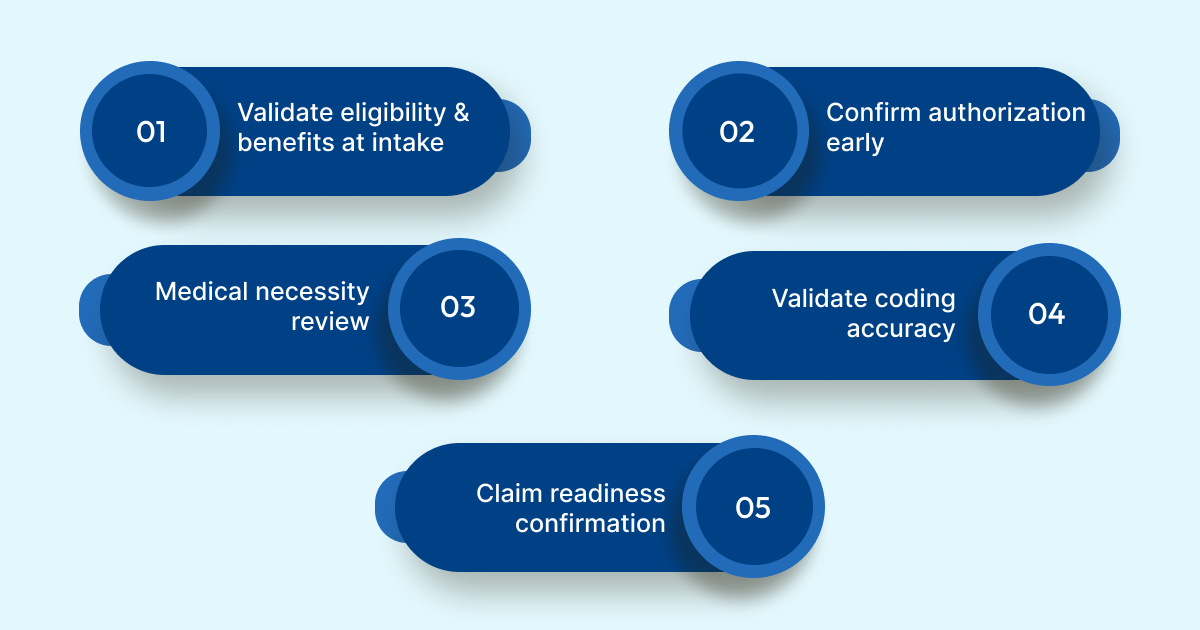
1. Validate eligibility and benefits at intake: Real-time eligibility verification confirms active coverage, benefit limits, network status, and secondary insurance. This prevents denials tied to inactive coverage and coordination of benefits errors.
2. Confirm authorization and referral requirements early: Authorization requirements should be identified before scheduling or delivering care. Early validation ensures approvals match the service, provider, and place of care.
3. Review documentation for medical necessity gaps: Medical necessity denials often stem from missing or unclear clinical details. Reviewing documentation before coding helps identify gaps in rationale or diagnosis-to-procedure linkage while they can still be addressed.
4. Validate coding accuracy and payer alignment: Pre-submission coding checks ensure diagnosis, procedure, and modifier combinations align with documentation and payer rules, including bundling and specificity requirements.
5. Confirm claim readiness before submission: A final readiness review brings eligibility, authorization, documentation, and coding together. Claims that fail validation can be corrected instead of sent prematurely.
At scale, manual checks are not sustainable. As claim volumes rise and payer logic grows more complex, automation becomes essential for consistent, early detection—shifting denial management from reactive recovery to proactive prevention.
How Automation Helps Prevent Claim Denials Before Submission
Automation moves denial prevention upstream. Instead of fixing issues after claims are rejected, AI-driven systems surface risk while claims are still being prepared, when corrections are faster and less costly.
- Context-aware medical coding with auditability: AI-powered coding analyzes full clinical documentation to assign ICD-10, CPT, HCPCS, and HCC codes consistently. Each coding decision is supported by an audit trail, helping teams maintain accuracy while meeting compliance requirements.
- Pre-submission payer rule validation: Automation applies payer-specific logic before claims are sent, checking authorization requirements, bundling rules, modifier usage, coverage alignment, and filing constraints. Catching these issues early reduces first-pass denials without adding manual review cycles.
- Documentation gap detection: Natural language processing identifies missing or unclear elements tied to medical necessity. Addressing these gaps while the encounter is still recent avoids retrospective addenda and reduces appeal volume.
- Workflow-level integration: When embedded into EHR and revenue cycle systems, automation works within existing workflows. Eligibility checks, coding validation, and documentation review happen in real time, without creating parallel processes or tool fatigue.
As chart volumes grow and payer logic becomes more complex, manual processes no longer scale. AI-powered automation enables consistent, pre-submission validation, reducing reliance on post-denial appeals while improving accuracy and compliance across the revenue cycle.
Platforms like RapidClaims apply this approach through autonomous medical coding and AI-driven risk adjustment, operating directly within EHR workflows to identify denial risk before claims are submitted.
How RapidClaims Improves Insurance Claim Reimbursement
RapidClaims is an AI-powered platform that reduces preventable claim denials by automating medical coding and validating claims against payer rules before submission. It improves reimbursement accuracy, shortens A/R cycles, and supports compliance with evolving coding and regulatory standards.
- Explainable, audit-ready AI: Every code is assigned with a complete audit trail, ensuring transparency and compliance with ICD-10, CPT, HCPCS, and E&M guidelines.
- Configurable, payer-aware rule sets: Coding logic is customized by specialty and automatically updated to reflect payer policies, NCCI edits, and LCD/NCD requirements.
By combining autonomous coding with real-time validation, RapidClaims enables faster, more predictable reimbursement while reducing administrative effort.

Conclusion
Denied insurance claims are not random. They arise from predictable gaps in eligibility checks, documentation quality, coding accuracy, and payer rule enforcement. When left unaddressed, these gaps increase rework, delay reimbursement, and elevate compliance risk.
As payer scrutiny intensifies and claim volumes rise, clarity around what are the reasons for denied claims becomes essential for protecting cash flow, shortening revenue cycles, and maintaining compliance. AI-powered platforms like RapidClaims support this shift by embedding accuracy, validation, and payer-aware controls directly into medical coding and claims workflows.
Reach out to us to see how we can help improve claim acceptance rates and reimbursement performance.
FAQs
1. Why do claims get denied?
Claims are denied when the submitted data, documentation, or coding does not meet payer requirements. Common causes include eligibility issues, missing authorization, coding errors, and insufficient documentation.
2. Which is an example of a common reason for a denied claim?
A frequent example is submitting a claim without the required prior authorization for a procedure. Even when the service is medically necessary, missing approval often leads to denial.
3. What are the common reasons for denials?
The most common reasons include coding inaccuracies, documentation gaps, eligibility errors, lack of prior authorization, and violations of payer-specific rules.
4. Which denials are easiest to prevent?
Eligibility errors, missing documentation, and many coding mismatches are among the easiest to prevent. These issues can often be detected before submission with automated checks.
5. Can denied claims be prevented before submission?
Yes. Pre-submission validation of eligibility, authorization, coding, and documentation can prevent many denials before claims reach the payer.
6. How does automation improve claim acceptance rates?
Automation validates codes, documentation, and payer-specific rules in real time. This reduces first-pass denials and limits manual rework.
7. Can AI reduce denials related to medical necessity?
AI can flag documentation gaps and coding inconsistencies that affect medical necessity decisions, though final clinical judgment remains essential.
.png)
Mary Degapogu
Mary Degapogu is a proficient medical coder with 6 years of experience in E/M Outpatient and ED Profee coding, focused on precise code assignment and documentation compliance to drive clean claims and revenue integrity at RapidClaims.
Latest Post
expert insights with our carefully curated weekly updates
Related Post
Top Products

%201.png)
.jpg)
.jpg)






