Benefits of Electronic Medical Records: How EHRs Improve Care and Revenue

Healthcare organizations generate enormous volumes of clinical and administrative data every day. When that data sits in fragmented systems or paper charts, it slows care delivery, weakens documentation, and creates steady revenue leakage through coding errors and avoidable claim denials. At this point, electronic medical records are no longer just a compliance requirement. They are operationally critical.
Nearly 88% of office-based physicians now use EHR or EMR systems, but adoption alone does not guarantee results. Without effective use, organizations still face delayed charts, documentation gaps, and revenue cycle risk. When implemented and operationalized correctly, electronic medical records improve documentation quality, support regulatory compliance, and create the structured data foundation needed for accurate coding, faster reimbursements, and audit-ready operations.
As EHRs become embedded across clinical, compliance, and billing workflows, the real differentiator is how well organizations turn EHR data into action.
Here, we break down the practical benefits of electronic medical records and their direct impact on care quality, financial performance, and operational scale.
Key Takeaways
- Electronic medical records improve care and revenue by standardizing documentation, supporting accurate coding, and reducing claim denials across clinical and billing workflows.
- Clean, structured EMR data strengthens revenue cycle performance, enabling faster chart completion, better medical necessity validation, and more predictable reimbursements.
- Patient care benefits from EMRs through safer decisions, fewer medication errors, better care coordination, and stronger data security.
- When paired with AI automation like RapidClaims, EMRs deliver greater accuracy at scale by closing documentation gaps, improving HCC capture, and accelerating compliant billing.
Table of Contents
- What Are Electronic Medical Records and How Do They Work?
- Key Challenges Electronic Medical Records Are Designed to Solve
- Benefits of Electronic Medical Records for Patients
- Benefits of Electronic Medical Records for Healthcare Providers
- How Electronic Medical Records Improve Revenue Cycle Performance
- Real-World Use Cases of Electronic Medical Records
- Best Practices for Implementing Electronic Medical Records Effectively
- Limitations and Risks of Electronic Medical Records
- Conclusion
- Frequently Asked Questions (FAQs)
What Are Electronic Medical Records and How Do They Work?
Electronic medical records are digital systems that store and manage patient clinical information across care encounters. Although EMR and EHR are often used interchangeably, EMRs traditionally focus on records within a single organization, while EHRs enable data sharing across care settings. Most modern systems support both.
EMRs organize patient data in structured formats that can be updated, accessed, and audited over time. This structure supports clinical decision-making and also ensures documentation is usable for coding, compliance, and revenue cycle workflows.
Core EMR components include:
- Structured clinical notes and encounter documentation
- Diagnoses, procedures, and problem lists aligned with ICD-10, CPT, HCPCS, and HCC models
- Medication, allergy, lab, and imaging records
- Audit trails and access logs
- Secure data exchange through HL7 and FHIR standards
By standardizing how clinical data is captured and exchanged, electronic medical records create a reliable data foundation for interoperability and automation across coding, billing, and analytics systems. To understand their value, it’s important to examine the specific challenges EMRs are designed to address across clinical and financial workflows.
Key Challenges Electronic Medical Records Are Designed to Solve
Many healthcare organizations struggle to realize the full value of their EMR investments due to fragmented records, inconsistent documentation, and disconnected workflows. These issues affect both clinical operations and the revenue cycle.
Paper-based records and siloed systems slow access to patient information, delay documentation, and leave coders working with incomplete charts. Billing teams then face the downstream impact in the form of rework, denials, and delayed reimbursements.
These breakdowns typically result in:
- Coding inaccuracies caused by unclear or missing documentation
- Delays between care delivery and chart completion
- Slower coding and billing cycles due to manual follow-ups
- Higher denial rates are tied to medical necessity gaps
- Increased audit exposure under CMS and payer-specific requirements
What begins as a documentation problem quickly becomes a financial one. Delayed charts, slow coding, slow claim submission, and extending days in accounts receivable.
This operational complexity is also reshaping workforce needs. According to the U.S. Bureau of Labor Statistics, roles related to medical records and health information management are projected to grow 15% by 2034, reflecting the healthcare system’s increasing dependence on structured data to support compliance, analytics, and revenue cycle workflows.
Electronic medical records address these challenges by standardizing data capture and centralizing patient information into a single source of truth, enabling documentation to support clinical care, coding accuracy, and financial performance.
Also Read: Common Types and Usage of Medical Coding Examples
Benefits of Electronic Medical Records for Patients
Electronic medical records improve the patient experience by making care safer, more coordinated, and easier to navigate across providers and care settings.
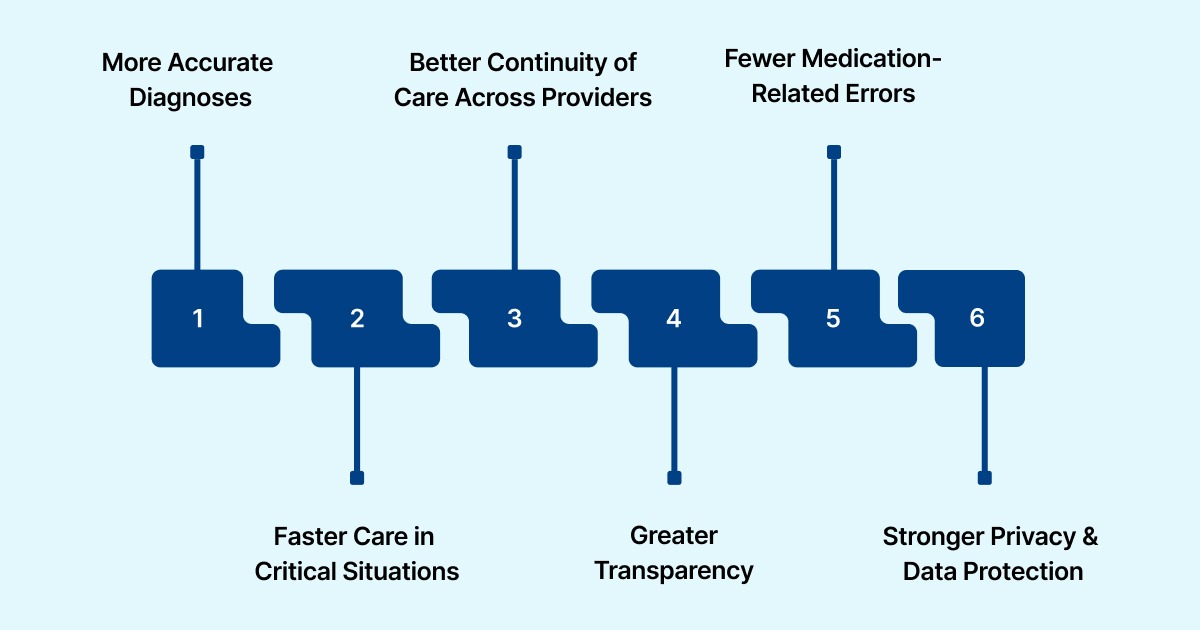
Below are the core benefits of electronic medical records:
1. More Accurate Diagnoses and Treatment
EHRs consolidate a patient’s complete medical history into a single longitudinal record.
- Clinicians can review diagnoses, medications, lab results, imaging, allergies, and prior treatments in one place
- Reduces reliance on fragmented or incomplete information
- Supports more accurate diagnoses and better-informed treatment decisions
2. Faster Care in Critical Situations
Immediate access to patient data is essential in emergencies.
- Emergency teams can quickly view allergies, chronic conditions, and active medications
- Care decisions are not delayed when patients are unconscious or unable to communicate
- Reduces the risk of adverse reactions during urgent treatment
3. Better Continuity of Care Across Providers
Patients often receive care from multiple providers and facilities.
- Shared records ensure all providers work from the same information
- Reduces duplicate tests and conflicting treatments
- Improves follow-up care and long-term condition management
Industry surveys show that around 45% of patients report improved care quality after EHR adoption, highlighting the role of digital records in patient safety and consistency.
4. Greater Transparency and Patient Engagement
Patient portals linked to EHRs improve visibility into care.
- Patients can access test results, visit summaries, prescriptions, and care plans
- Encourages informed questions and shared decision-making
- Helps patients better manage chronic conditions
5. Fewer Medication-Related Errors
Electronic prescribing reduces common sources of error.
- Eliminates issues caused by illegible handwriting
- Flags duplicate prescriptions and allergy conflicts
- Surfaces alerts at the point of care
Given the high cost of medical errors across the healthcare system, reducing medication-related inaccuracies has both clinical and financial impacts.
6. Stronger Privacy and Data Protection
EHRs offer more robust security than paper-based records.
- Role-based access controls limit who can view patient data
- Encryption and audit trails protect sensitive information
- Supports compliance with privacy and data protection regulations

Benefits of Electronic Medical Records for Healthcare Providers
For healthcare organizations, electronic medical records serve as foundational systems that support clinical quality, operational efficiency, and financial performance.
1) Real-Time Access to Complete Patient Data
EHRs give clinicians immediate access to patient histories, medications, lab results, and prior encounters.
- Reduces time spent searching for records
- Limits duplicate testing and unnecessary procedures
- Enables faster, more confident clinical decisions
2) Improved Care Coordination Across Teams
Shared records allow care teams to collaborate using a single source of truth.
- Aligns physicians, nurses, specialists, labs, and administrative staff
- Improves handoffs and reduces communication gaps
- Supports coordinated care across departments and locations
3) Clinical Decision Support and Safety Controls
Modern EHRs embed safeguards directly into clinical workflows.
- Alerts for medication interactions and allergy risks
- Prompts for abnormal results or missing documentation
- Supports adherence to evidence-based guidelines
4) Reduced Paperwork and Administrative Burden
Digital documentation replaces manual, paper-based processes.
- Eliminates paper charts, transcription, and physical storage
- Reduces repetitive data entry
- Tools like voice input and ambient documentation lower the clinician workload
5) Stronger Documentation and Compliance Posture
Structured documentation improves consistency and accuracy.
- Supports reliable ICD-10, CPT, and HCC coding
- Strengthens medical necessity documentation
- Improves audit readiness for CMS and commercial payers
6) Improved Revenue Cycle Performance
Documentation quality directly affects reimbursement outcomes.
- Faster chart completion and coding turnaround
- Higher first-pass claim acceptance rates
- Fewer denials, rework, and payment delays
7) Scalability and Operational Efficiency
EHRs help organizations grow without increasing complexity.
- Standardized workflows across specialties and locations
- Supports higher patient volumes without proportional administrative growth
- Enables consistent operations at scale
8) Actionable Data For Analytics and Population Health
Structured EHR data supports data-driven decision-making.
- Enables quality reporting and performance monitoring
- Helps identify care gaps and risk trends
- Supports population health and value-based care initiatives using real-time insights
Many of these operational improvements extend directly into the revenue cycle. Documentation quality, workflow consistency, and data accessibility all play a critical role in how accurately and efficiently healthcare organizations are reimbursed.
Also Read: EMR Conversion Challenges & Best Practices in 2026
How Electronic Medical Records Improve Revenue Cycle Performance
Electronic medical records directly influence revenue cycle outcomes by improving documentation quality and coding accuracy. When EMR data is structured, timely, and integrated with downstream systems, claims move faster, and denial risk decreases.
EMRs strengthen revenue workflows by capturing diagnoses and procedures at the point of care and applying documentation standards before charts are finalized. This ensures records are ready for coding earlier and reduces delays caused by follow-up queries or missing information.
With clean, structured EMR data flowing into coding and validation tools, organizations can:
- Shorten chart completion and coding timelines
- Confirm medical necessity before claim submission
- Reduce denials tied to documentation gaps
- Improve HCC capture and RAF score accuracy
- Accelerate billing cycles and cash flow
For Medicare Advantage populations, documentation specificity is especially critical. Missed or vague diagnoses translate directly into lost risk-adjusted revenue.
To take this further, AI-driven platforms like RapidClaims help activate EMR data for accuracy at scale. RapidClaims works alongside your EHR to automate coding, surface documentation gaps in real time, and support compliant risk adjustment. This reduces manual effort, improves claim acceptance rates, and keeps coding and billing workflows accurate without adding operational complexity.
Real-World Use Cases of Electronic Medical Records
Electronic medical records serve as the foundation for standardized workflows, automation, and consistent financial performance across healthcare organizations.
- Hospital Systems: Large hospitals use EMRs to standardize documentation across departments. This reduces duplicate testing, improves coding accuracy, lowers denial rates, and supports faster claim submission through clean, structured data.
- Physician Groups: Multi-provider practices rely on EMRs to maintain consistent documentation at scale. Structured charting speeds chart completion, reduces administrative burden, and enables timely coding. In value-based care models, it also improves HCC capture and reimbursement accuracy.
- Medical Billing Organizations: Billing teams integrate EMR data directly into coding and validation systems to eliminate manual chart review. This increases coder productivity and allows billing operations to scale without increasing headcount while maintaining compliance.
Across these use cases, EMRs create operational consistency by ensuring clinical data is accurate, accessible, and usable across coding, compliance, and revenue workflows. Their impact depends on reliable data quality and system integration.
Also Read: How Healthcare Reimbursement Works: 3 Key Steps Explained
Best Practices for Implementing Electronic Medical Records Effectively
Effective EMR implementation goes beyond technology deployment. Organizations that achieve meaningful clinical and financial impact approach EMRs as an operational transformation, not an IT project.
Key best practices include:
1. Establish Clear Governance and Ownership: Define accountability across clinical, IT, compliance, and revenue cycle teams to keep documentation standards, system configuration, and performance goals aligned.
2. Use a Phased Rollout Strategy: Pilot EMR workflows within selected specialties before scaling organization-wide. This allows teams to refine templates, workflows, and integrations while minimizing disruption and revenue risk.
3. Focus Training on Real Workflows: Train clinicians and coders on how documentation decisions affect coding accuracy, reimbursement, and audit readiness, rather than limiting training to system navigation.
4. Align Templates with Coding and Compliance Needs: Configure EMR templates to support ICD-10, CPT, HCC, and payer-specific documentation requirements to reduce rework and denials.
5. Integrate EMRs with Downstream Systems: Connect EMRs with coding, risk adjustment, and analytics platforms to enable real-time validation and operational visibility.
6. Monitor Performance Continuously: Track KPIs such as clean claim rate, denial trends, and chart turnaround time using parallel coding and post-go-live audits to identify issues early.
7. Optimize After Go-Live: Treat implementation as ongoing. Regular reviews and incremental improvements ensure EMRs continue to support both clinical quality and financial performance.
Even with strong implementation practices, EMRs introduce operational risks that must be actively managed. Understanding these limitations helps organizations set realistic expectations and put the right controls in place.
Limitations and Risks of Electronic Medical Records
Electronic medical records provide significant clinical and operational benefits, but their effectiveness depends on disciplined implementation and ongoing governance. Most risks stem from process, integration, and usage gaps rather than the technology itself.
Common challenges include:
- Ongoing Record Maintenance: Patient records must be updated after every encounter. Because documentation is contributed by multiple teams, delays or inaccuracies can affect care decisions, coding accuracy, and reimbursement.
- Incomplete or Fragmented Information: Poor integration with external systems, summarized patient portals, or delayed data exchange can create temporary gaps, limiting a complete clinical view and increasing manual reconciliation.
- Data Security and Privacy Risks: Although EMRs include encryption, access controls, and audit logs, security depends on user behavior. Shared credentials, unattended workstations, or weak policy enforcement increase exposure.
- System Availability and Reliability Issues: Power outages, network disruptions, or limited device access can interrupt record availability if downtime procedures are not well defined.
- Integration and Standardization Challenges: Variations in data formats, workflows, and system configurations can limit interoperability and reduce efficiency across care, coding, and billing processes.
- Change Management and Training Demands: Without proper training and workflow alignment, EMRs can increase clinician burden, leading to workarounds and inconsistent documentation.
These challenges are manageable with the right approach. Early involvement of clinical, coding, IT, and compliance teams, phased rollouts, clear ownership of documentation standards, and continuous monitoring of data quality and user feedback are essential to sustaining long-term EMR value.
This is where platforms like RapidClaims help bridge the gap. RapidClaims builds on your existing EMR by applying AI-driven medical coding automation that identifies documentation gaps, validates coding in real time, and enforces payer and regulatory rules.
Instead of adding complexity, RapidClaims helps you turn EMR data into actionable insights, reducing denials, improving reimbursement accuracy, and supporting both financial performance and care quality.

Conclusion
The benefits of electronic medical records go far beyond replacing paper charts. When implemented with clear standards and integrated into downstream workflows, EMRs improve documentation quality, support compliant coding, and reduce claim denials.
Fragmented records slow revenue cycles and increase compliance risk. EMRs, by contrast, create a structured data foundation for accurate coding, faster claim submission, and audit-ready operations at scale.
When paired with automation, platforms like RapidClaims extend EMR value by identifying documentation gaps early, validating claims in real time, and improving reimbursement accuracy without disrupting clinical workflows.
Contact us to strengthen your coding, reduce denials, and accelerate reimbursements.
Frequently Asked Questions (FAQs)
1. What are the benefits of an electronic medical record?
Electronic medical records improve documentation accuracy, speed up chart completion, and support safer clinical decisions. They also reduce administrative overhead and strengthen coding and billing workflows.
2. What are five common functions of EHR systems?
EHRs support clinical documentation, diagnosis and procedure capture, medication and allergy tracking, lab and imaging results, and secure data exchange across systems.
3. What are the advantages and disadvantages of electronic records?
Advantages include better data accessibility, improved care coordination, and stronger compliance. Disadvantages typically relate to implementation challenges, training needs, and integration complexity rather than the technology itself.
4. What is the difference between an EHR and an EMR?
An EMR is a digital patient record used within a single organization. An EHR extends this by enabling data sharing across providers, systems, and care settings.
5. Do hospitals use EHR or EMR systems?
Hospitals primarily use EHR systems because they support interoperability, multi-department workflows, and data exchange across care settings.
6. How do electronic medical records reduce claim denials?
EMRs improve documentation completeness and consistency, helping ensure claims meet medical necessity and payer-specific requirements before submission.

Rejones Patta
Rejones Patta is a knowledgeable medical coder with 4 years of experience in E/M Outpatient and ED Facility coding, committed to accurate charge capture, compliance adherence, and improved reimbursement efficiency at RapidClaims.
Latest Post
expert insights with our carefully curated weekly updates
Related Post
Top Products

%201.png)
.jpg)
.jpg)






