Types of AI in Healthcare: Applications Across Clinical and Revenue Workflows

AI is now a core part of modern healthcare operations. Machine learning and related technologies are helping healthcare organizations apply data-driven intelligence across clinical, administrative, and revenue workflows. When implemented correctly, AI reduces operational friction, improves accuracy, and supports better care delivery.
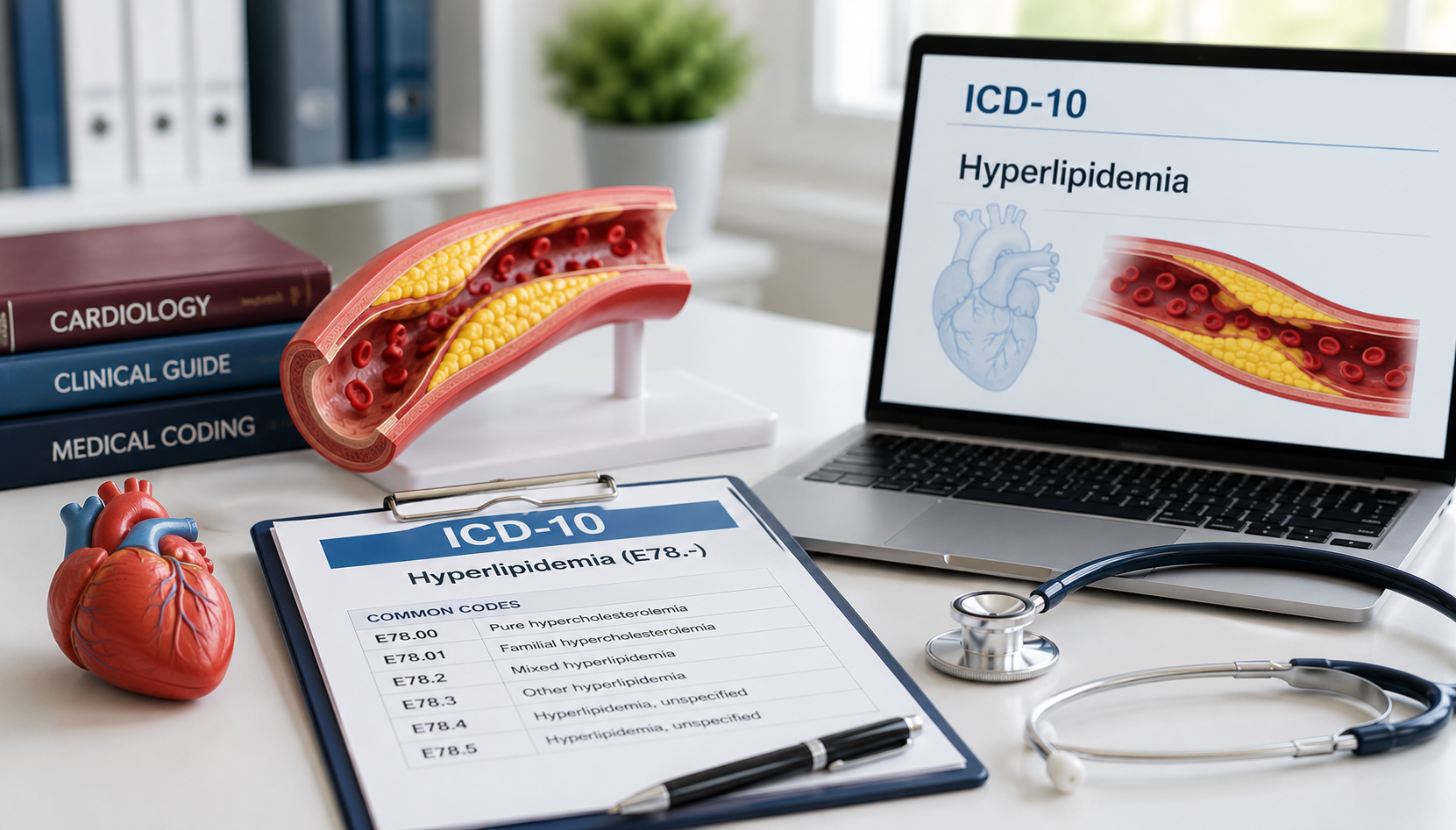
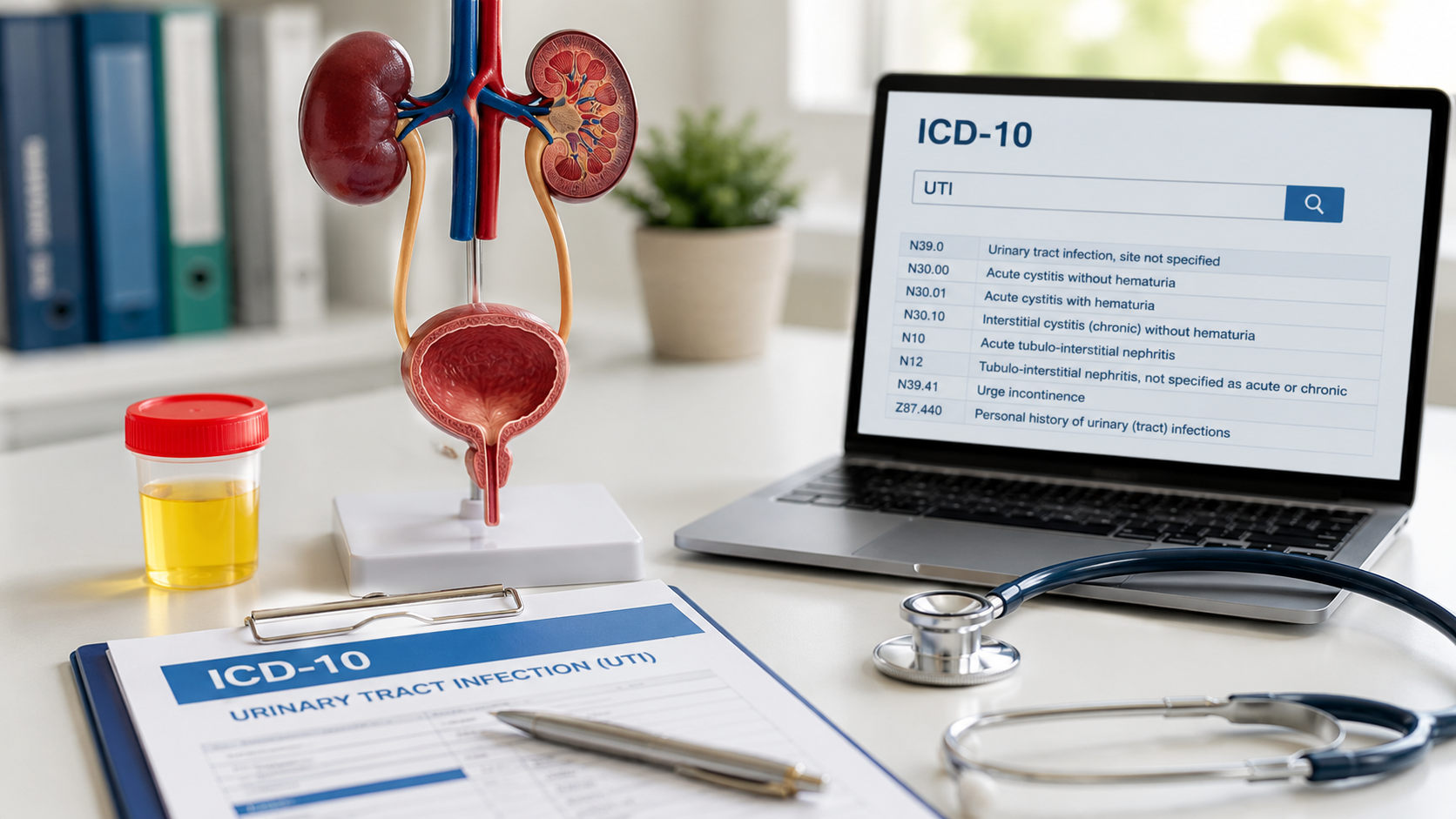
Nearly 80% of medical data is unstructured, scattered across clinical notes, registries, and diagnostic images such as CT scans, MRIs, and X-rays. As healthcare systems approach 2,000 exabytes of data generated each year, traditional tools can no longer keep pace, making AI essential rather than optional.
For healthcare leaders today, the question is no longer whether to adopt AI, but where it can deliver measurable impact across clinical care, medical coding, and revenue operations.
This article breaks down the core types of AI in healthcare and explains how they are being applied across care delivery, documentation, and revenue cycle workflows.
Key Takeaways
- Types of AI in healthcare include machine learning, deep learning, NLP, rule-based systems, and RPA, each supporting specific clinical, operational, and revenue cycle workflows.
- AI is already improving diagnostics, documentation, medical coding, and denial prevention by reducing manual effort and enabling earlier, more accurate decisions.
- The greatest value comes when AI is embedded into existing workflows with strong governance, auditability, and human oversight.
- Platforms like RapidClaims apply these AI capabilities directly to medical coding and revenue operations, helping organizations improve accuracy, reduce denials, and scale efficiently.
Table of Contents
- The Growing Role of AI in Healthcare Operations
- Core Types of Artificial Intelligence in Healthcare
- How AI Is Applied Across Healthcare Workflows
- How AI Improves Revenue Cycle Performance
- How to Implement AI for Medical Coding and Revenue Teams
- The Future of AI in Healthcare
- How RapidClaims Applies AI in Real-World Healthcare Workflows
- Conclusion
- FAQs
The Growing Role of AI in Healthcare Operations
Healthcare organizations are operating under sustained pressure. Rising costs, workforce shortages, and growing administrative complexity are straining both care delivery and revenue operations. Clinicians are spending more time on documentation, coding, and billing, leaving less time for direct patient care.
AI is beginning to address these structural challenges in practical ways:
- Automating administrative workflows such as documentation, coding, and billing
- Supporting earlier disease detection and patient prioritization
- Improving accuracy across clinical and financial processes
As a result, care teams can focus more on decision-making and less on manual work.
Industry data underscores the urgency. The Philips Future Health Index 2025 reports that extended wait times are already contributing to poorer patient outcomes, while global projections indicate a potential shortage of up to 11 million healthcare workers by 2030. These pressures make efficiency gains essential, not optional.
Meeting these demands requires more than a single tool. Healthcare organizations increasingly rely on multiple forms of AI, each designed to address specific clinical, operational, and revenue challenges at scale.
7 Types of Artificial Intelligence in Healthcare
Healthcare AI is not a single system. It is a set of specialized technologies designed to process structured and unstructured data, identify patterns, and support decisions across clinical, operational, and revenue workflows. Most organizations deploy multiple AI approaches together, with each addressing a specific layer of complexity.
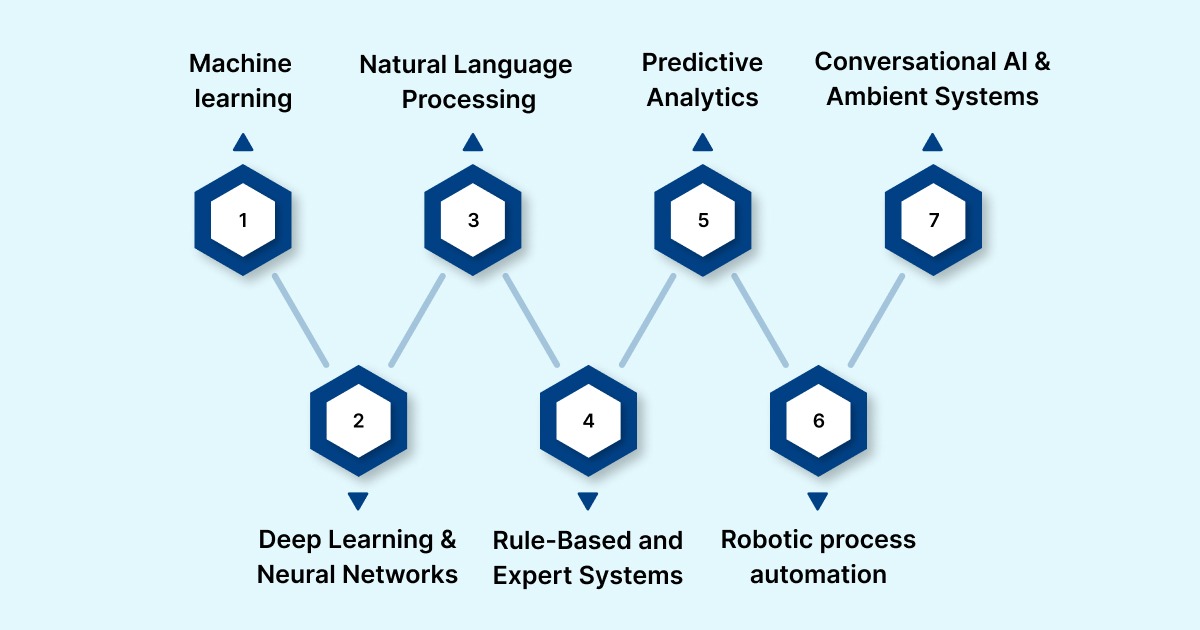
1. Machine learning (ML)
Machine learning models analyze historical healthcare data and apply learned patterns to new cases. These models primarily work with structured data such as diagnosis codes, procedure codes, claims history, utilization metrics, and payer outcomes.
Common uses include:
- Predicting claim denial likelihood before submission
- Identifying coding inconsistencies across similar encounters
- Classifying encounters by clinical or financial complexity
- Prioritizing high-risk or high-value claims for review
As more validated outcomes are incorporated, model accuracy improves, making ML particularly effective in revenue cycle workflows.
2. Deep Learning and Neural Networks
Deep learning is a subset of machine learning that uses multi-layer neural networks to process complex, high-dimensional data. It is well-suited for unstructured and sequential inputs where traditional rule-based logic is insufficient.
Key applications include:
- Medical imaging and pathology analysis
- Speech recognition for clinical documentation
- Pattern recognition across longitudinal patient records
Operationally, deep learning often supports upstream documentation capture and interpretation that directly influences coding accuracy, risk adjustment, and reimbursement.
3. Natural Language Processing (NLP)
Natural language processing enables systems to interpret and structure human language found in clinical documentation, including physician notes, discharge summaries, operative reports, and nursing documentation.
NLP supports healthcare automation by:
- Extracting diagnoses, conditions, and procedures from free-text notes
- Identifying the missing specificity required for ICD-10, CPT, and HCC coding
- Detecting documentation gaps or ambiguous language
- Normalizing documentation across providers and specialties
By converting unstructured text into structured, codable data, NLP reduces manual chart review and improves downstream audit readiness.
4. Rule-Based and Expert Systems
Rule-based systems apply predefined logic derived from clinical guidelines, payer policies, and regulatory standards. These systems do not learn from data, but they provide consistency and transparency.
They are critical for:
- Enforcing NCCI edits, LCDs, and NCDs
- Applying payer-specific coding and medical necessity rules
- Supporting compliance checks and audit workflows
Rule-based systems are often paired with machine learning models to combine interpretability with predictive intelligence.
5. Predictive Analytics and Time-Series Models
Predictive analytics uses statistical and machine learning techniques to forecast future outcomes using historical and real-time data.
Typical healthcare use cases include:
- Denial trend forecasting
- Revenue leakage detection
- Risk adjustment and RAF performance monitoring
- Utilization and capacity planning
These models enable earlier intervention in workflows, reducing downstream clinical and financial risk.
6. Robotic process automation (RPA)
Robotic process automation handles repetitive, rules-based tasks by mimicking human interactions with software systems. RPA does not make probabilistic decisions and is typically used alongside AI models.
Healthcare applications include:
- Eligibility and benefits verification
- Claim submission and status tracking
- Routing exceptions to appropriate teams
RPA provides scale and consistency, while AI models handle interpretation, prioritization, and decision support.
7. Conversational AI and Ambient Systems
Conversational AI includes voice-based and text-based systems that support interactions and documentation. In clinical environments, this often takes the form of ambient documentation tools that capture encounters in real time.
These systems improve downstream workflows by:
- Enhancing documentation completeness
- Reducing clinician documentation burden
- Improving data quality for feeding coding and billing systems
Together, these AI technologies form the foundation of modern healthcare automation. Their impact is greatest when deployed in coordination across clinical documentation, compliance, and revenue cycle workflows, supported by strong governance and human oversight.
How AI Is Applied Across Healthcare Workflows
AI is already applied across healthcare, delivering measurable impact in clinical care, research, and operations. Its value is most visible where it reduces manual effort, enables earlier intervention, and scales complex workflows without compromising accuracy or compliance. Below are the most practical and widely adopted applications today.
1. Clinical Care and Diagnostics
AI supports earlier and more consistent diagnosis across oncology, neurology, cardiovascular care, and other specialties.
Key applications include:
- Early disease detection using ML and deep learning models trained on large clinical datasets
- Diagnostic decision support to reduce variability and missed findings
- Medical imaging analysis across X-rays, CT scans, MRIs, and pathology slides
- Case prioritization for urgent or high-risk patients
These tools act as clinical support systems, improving consistency while keeping clinicians in control.
2. Patient Monitoring and Risk Stratification
AI enables continuous monitoring and earlier intervention by analyzing real-time patient data.
Common use cases include:
- Detection of early deterioration risks such as sepsis or respiratory failure
- Risk stratification for readmissions and chronic disease complications
- Proactive intervention planning based on predictive insights
- Population-level monitoring across acute and chronic care settings
This allows care teams to intervene earlier and allocate resources more effectively.
3. Personalized Treatment Planning
AI supports more individualized care by combining multiple data sources.
Where it adds value:
- Therapy response prediction using clinical history and genomics
- Treatment selection optimization in oncology and pharmacogenomics
- Reduced adverse drug reactions through better patient–drug matching
- Support for complex and chronic care planning
Personalization improves outcomes while reducing unnecessary trial-and-error treatment.
4. Clinical Documentation and Decision Support
AI is increasingly used to reduce documentation burden and improve data quality.
Key capabilities include:
- Ambient documentation capturing clinician–patient conversations
- Automated transcription and structured EHR summaries
- Improved completeness and consistency of clinical records
- Stronger downstream data quality for coding and billing workflows
This frees clinicians to focus more on patient care without sacrificing documentation quality.
5. Research and Drug Discovery
AI accelerates biomedical research and early-stage drug development.
Primary applications include:
- Modeling biological systems and disease pathways
- Screening and prioritizing drug candidates at scale
- Predicting efficacy and safety earlier in the pipeline
- Shortening the time from discovery to clinical trials
These capabilities reduce development timelines and research costs, especially for complex diseases.
6. Robotics and Assisted Procedures
AI-powered robotics enhance precision in surgical environments.
Clinical benefits include:
- Support for minimally invasive and complex procedures
- Motion stabilization and enhanced visualization
- Reduced complication rates and recovery times
- More consistent surgical outcomes
Robotic systems assist surgeons without replacing human control.
7. Administrative Workflows
AI is widely adopted in administrative and financial operations where data volume and repetition are high.
Revenue cycle applications include:
- Automated medical coding using NLP for ICD-10, CPT, HCPCS, and HCC
- Claim validation and pre-submission scrubbing against payer rules
- Denial prediction and root-cause analysis before submission
- Clinical documentation improvement for compliant coding
- Risk adjustment and RAF accuracy improvement
These examples show how AI delivers real-world value in healthcare. When aligned with existing workflows and supported by governance and human oversight, AI improves accuracy, efficiency, and scalability without replacing clinical or operational judgment.

How AI Improves Revenue Cycle Performance
AI fits naturally into healthcare revenue cycle management, where teams often face fragmented systems, unclear priorities, and high claim volumes. These constraints make consistent revenue recovery difficult at scale.
Applied across the revenue cycle, AI helps:
- Prioritize the right claims by identifying high-risk or high-value submissions based on payer behavior and historical outcomes
- Reduce manual effort by automating claim validation, documentation checks, and exception routing
- Improve follow-up efficiency by recommending timely actions based on claim status and payer response patterns
The result is a more focused, efficient revenue cycle with fewer delays and less operational strain.
Clinical and revenue workflows are tightly linked. More accurate documentation and earlier condition capture directly improve code selection, HCC assignment, and reimbursement accuracy. When clinical AI strengthens data quality upstream, revenue performance improves downstream.
How to Implement AI for Medical Coding and Revenue Teams
Implementing AI in healthcare operations requires a structured approach. Teams that see consistent results follow a clear, phased sequence rather than treating AI as a plug-and-play tool.
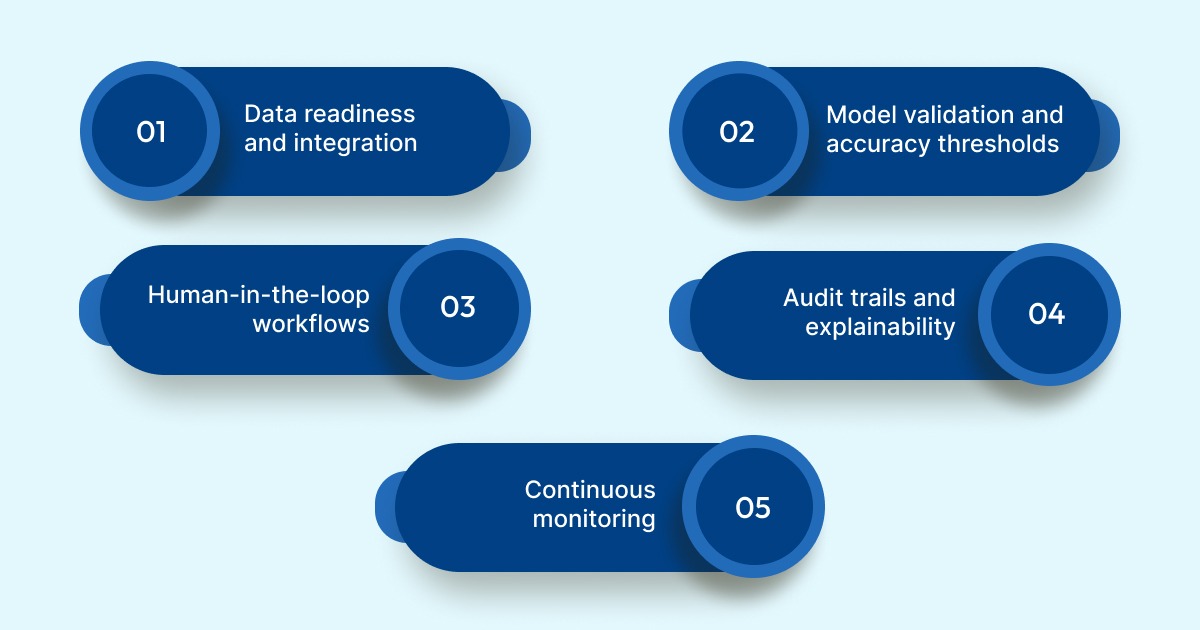
1. Data readiness and integration: Start with clean, reliable EHR data. Standardize clinical terminologies and establish secure integrations using HL7 or FHIR to ensure AI systems receive accurate, usable inputs.
2. Model validation and accuracy thresholds: Define acceptable accuracy levels for coding, risk prediction, and validation tasks. Test AI outputs against historical charts before deploying models in live workflows.
3. Human-in-the-loop workflows: Design workflows where coders, auditors, and compliance teams review and approve AI-generated outputs. AI should support decisions, not replace accountability.
4. Audit trails and explainability: Ensure every AI-assisted action is traceable. Maintain clear logs that show data sources, applied rules, and model confidence to support audits and regulatory requirements.
5. Continuous monitoring and retraining: Monitor performance as payer rules, coding standards, and documentation patterns evolve. Periodic retraining helps prevent model drift and maintains long-term accuracy.
As organizations mature their AI deployments, focus is shifting from initial adoption to long-term governance, scalability, and how these systems will continue to evolve within healthcare operations.
The Future of AI in Healthcare
AI is moving healthcare beyond isolated efficiency gains toward system-wide impact across care delivery, operations, and research. McKinsey estimates generative AI could contribute $60 to $110 billion annually to the US healthcare system through improved efficiency, fewer errors, reduced readmissions, and better workforce utilization. It is also enabling new models such as personalized care and digital therapeutics.
Today's AI systems remain task-specific. Most fall under artificial narrow intelligence (ANI), built for defined functions like image analysis, data extraction, or prediction. While artificial general intelligence (AGI) is an area of ongoing research, it is not yet relevant to real-world healthcare workflows.
What matters now is execution. Health systems are already using AI to streamline administrative work, support documentation, analyze imaging data, and assist clinical decision-making. These applications reduce routine errors and manual effort, allowing clinicians to focus on high-value, judgment-driven care.
As AI adoption expands, risk management becomes essential. Protecting patient data, ensuring model accuracy, and mitigating bias require strong governance, continuous validation, and human oversight.
Also Read: Top Vendors for Revenue Cycle Management in Healthcare
While many organizations struggle to operationalize these AI capabilities at scale, some platforms are purpose-built to apply them directly within revenue cycle workflows.
How RapidClaims Applies AI in Real-World Healthcare Workflows
RapidClaims is an AI-powered revenue cycle intelligence platform designed for healthcare organizations that need accuracy, scale, and compliance across coding and claims operations. The platform combines machine learning, NLP, and rules-based logic to automate routine work while preserving governance and audit control.
Key strengths of the RapidClaims platform:
- Human-in-the-loop design: AI automates routine analysis while coders and compliance teams retain final control
- EHR-native integration: Connects with existing systems using HL7 and FHIR standards
- Compliance-first architecture: Continuously updated payer rules and CMS guidelines
Core products and capabilities include:
RapidCode — Autonomous AI Medical Coding
- Uses NLP and machine learning to assign ICD-10, CPT, HCPCS, E&M, and HCC codes directly from clinical documentation
- Reduces manual chart review for routine encounters while maintaining transparent audit trails
- Scales high-volume coding without compromising accuracy or compliance
RapidCDI — Documentation and Risk Improvement
- Identifies missing specificity and documentation gaps at the point of care
- Improves HCC capture and E/M level accuracy
- Supports risk adjustment and value-based care by aligning documentation with reimbursement requirements
RapidScrub — Proactive Denials Prevention
- Applies predictive analytics and payer-specific rule logic before claim submission
- Catches common errors such as missing documentation, incorrect modifiers, and code mismatches
- Improves first-pass clean claim rates and reduces downstream rework
By embedding AI directly into coding, documentation, and claims workflows, RapidClaims helps healthcare teams reduce manual effort, prevent denials earlier, and improve financial performance without disrupting established operations.

Conclusion
Types of AI in healthcare play distinct but complementary roles, from structuring clinical documentation and predicting risk to enforcing compliance and improving financial accuracy. Their impact is greatest when these capabilities are applied together within governed, workflow-aware systems rather than in isolation.
As claim volumes rise and payer requirements evolve, manual coding and reactive denial management no longer scale. AI-driven platforms that combine natural language processing, machine learning, and payer-aware rules help healthcare organizations improve accuracy, reduce denials, and remain audit-ready without increasing operational burden.
RapidClaims brings these types of AI in healthcare into a single, operational platform built for real-world revenue cycle workflows, enabling coding and compliance teams to achieve measurable results with transparency and control.
Book a demo to see how RapidClaims supports compliant automation across the revenue cycle.
FAQs
1. What are the main types of AI used in healthcare?
Common AI types include machine learning, deep learning, natural language processing, generative AI, and robotic process automation. Each supports different clinical, operational, and revenue cycle workflows.
2. Which AI technologies are most effective for medical coding?
Natural language processing combined with supervised machine learning and payer-specific rule engines delivers the most reliable results for medical coding and validation workflows.
3. How does NLP improve coding accuracy?
NLP extracts structured clinical concepts from unstructured documentation, identifies missing specificity, and maps notes to ICD-10, CPT, and HCC requirements before claims are submitted.
4. Can AI replace certified medical coders?
No. AI reduces manual workload by automating routine cases, but certified coders remain responsible for complex scenarios, compliance review, and final coding decisions.
5. How does AI help reduce claim denials?
Predictive models flag high-risk claims before submission, while NLP identifies documentation gaps early. This allows corrective action before claims reach payers, reducing downstream rejections.
.png)
Mounika L
Mounika L is a skilled medical coder with 2 years of E/M Outpatient experience, specializing in accurate CPT, ICD-10, and HCPCS coding to ensure compliance and optimize reimbursement outcomes at RapidClaims.
Latest Post
expert insights with our carefully curated weekly updates
Related Post
Top Products

%201.png)