7 Types of Medicare Audits in Healthcare: What You Need to Know

Medicare audits are not routine administrative checks. They are built-in enforcement controls within federal reimbursement. Every claim submitted under Medicare Fee-for-Service or Medicare Advantage can be reviewed against CMS coverage rules, coding standards, and documentation requirements.
The financial impact is significant. Centers for Medicare & Medicaid Services (CMS) reported a 6.55% improper payment rate in FY 2025, representing nearly $28.83 billion in payments that did not fully comply with Medicare requirements. Unsupported diagnoses, incomplete documentation, or incorrect CPT and ICD-10 coding can trigger denials, extrapolated recoupments, payment suspension, and sustained regulatory scrutiny, even in the absence of fraud.
In this blog, we outline the types of Medicare audits, explain how they function, identify common triggers, and highlight practical steps revenue cycle teams can take to limit risk and safeguard reimbursement.
Key Takeaways
- Medicare audits are data-driven compliance reviews that evaluate documentation, coding accuracy, and adherence to CMS coverage rules across Fee-for-Service and Medicare Advantage claims.
- Common audit types include RAC, MAC, CERT, UPIC, SMRC, and TPE, each with different scopes, from improper payment recovery to fraud investigations.
- Most audits are triggered by billing outliers, documentation gaps, unsupported diagnoses, or coding inconsistencies, though some (like CERT) are randomly selected.
- Financial and operational impact can escalate quickly, especially when statistical sampling and extrapolation lead to large recoupment demands.
- Structured validation, continuous monitoring, and AI-powered coding automation reduce audit risk by strengthening documentation alignment and improving claim defensibility.
Table of Contents
- What Are Medicare Audits?
- The 7 Types of Medicare Audits
- How Medicare Audits Work: Process, ADRs, and Appeals
- Financial and Compliance Risks of Medicare Audits
- Common Findings in Medicare Audits
- How to Prepare for Medicare Audits
- How Automation Reduces Medicare Audit Risk
- How RapidClaims Strengthens Audit Readiness
- Conclusion
- FAQs
What Are Medicare Audits?
Medicare audits are structured reviews designed to confirm that submitted claims meet federal coverage, coding, and billing requirements. Auditors evaluate whether services were medically necessary, accurately coded, properly documented, and compliant with CMS policy.
For revenue cycle and compliance leaders, these reviews carry direct operational implications. Audit findings can disrupt cash flow, trigger recoupment demands, increase administrative burden, and elevate regulatory scrutiny. Even small documentation gaps can translate into financial exposure.
Although every audit centers on payment accuracy and compliance, the scope, methodology, and intensity of review vary depending on the contractor conducting the assessment. Let’s explore the types of Medicare audits in healthcare.
The 7 Types of Medicare Audits
Medicare audits are conducted by multiple contractors, each with a defined authority and review scope. While the objective remains payment accuracy and compliance, the methodology and enforcement intensity vary by audit type.
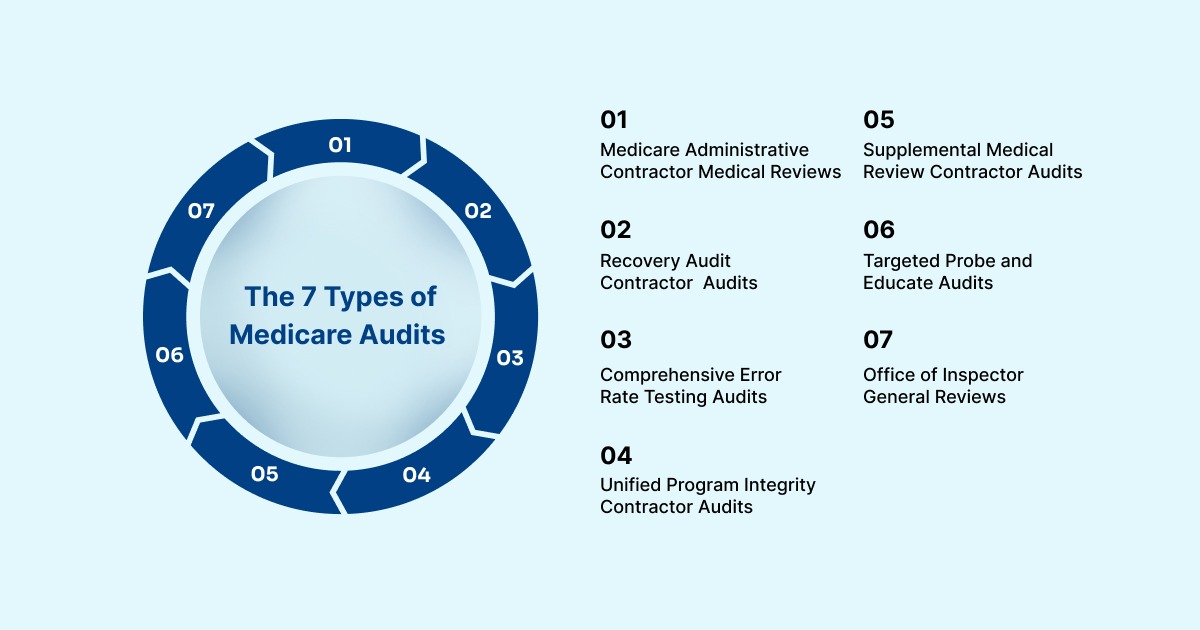
Below are the primary types of Medicare audits that revenue cycle and compliance leaders encounter.
1. Medicare Administrative Contractor (MAC) Medical Reviews
MACs process Medicare claims and conduct both pre-payment and post-payment reviews.
These audits typically assess:
- Documentation sufficiency
- Medical necessity
- CPT and ICD-10 alignment
- Compliance with LCD and NCD policies
Pre-payment reviews delay reimbursement until records are validated. Post-payment reviews may result in recoupment if documentation does not support the claim.
MACs also administer Targeted Probe and Educate (TPE) audits when providers demonstrate elevated error rates.
2. Recovery Audit Contractor (RAC) Audits
RACs identify and recover improper payments after claims have been paid. They rely heavily on data analytics to detect billing anomalies.
RAC reviews commonly focus on:
- Overpayments and underpayments
- Duplicate billing
- Incorrect coding patterns
- Medical necessity deficiencies
- NCCI edits violations
RAC audits frequently apply statistical sampling and extrapolation. When systemic documentation issues are identified, financial exposure may extend beyond the sampled claims.
3. Comprehensive Error Rate Testing (CERT) Audits
The CERT program measures the national improper payment rate for Medicare Fee-for-Service.
CERT audits evaluate:
- Coverage compliance
- Coding accuracy
- Billing rule adherence
- Documentation support
Claims are selected randomly. Although CERT primarily supports national reporting, insufficient documentation may still require repayment.
4. Unified Program Integrity Contractor (UPIC) Audits
UPIC audits investigate suspected fraud, waste, and abuse across Medicare and Medicaid programs.
These reviews may involve:
- Advanced data analytics
- Expanded documentation requests
- Provider interviews
- Site visits
- Escalation to payment suspension
UPIC audits represent elevated regulatory scrutiny and may lead to enforcement actions if significant irregularities are identified.
5. Supplemental Medical Review Contractor (SMRC) Audits
SMRC audits are issue-driven reviews directed by CMS and focus on high-risk service categories.
SMRC reviews typically examine:
- High-volume services
- High-cost procedures
- Claims with elevated error rates
- Billing trends flagged through CMS data analysis
These audits are national in scope and aligned with CMS program integrity priorities.
6. Targeted Probe and Educate (TPE) Audits
TPE audits are corrective reviews conducted by MACs for providers with high error rates or billing outliers.
The TPE process generally includes:
- Review of a limited claim sample
- Identification of recurring documentation or coding errors
- Structured provider education
- Follow-up review cycles
If performance does not improve after multiple rounds, the review may escalate.
7. Office of Inspector General (OIG) Reviews
The OIG conducts independent audits and investigations related to Medicare program integrity.
OIG reviews may include:
- Comprehensive compliance evaluations
- Financial audits
- Fraud investigations
- Enforcement referrals
OIG involvement signals significant regulatory risk and may result in civil penalties or exclusion from federal healthcare programs.
Each audit type differs in scope, but all ultimately assess documentation integrity, coding accuracy, and compliance with CMS coverage rules.
Understanding the contractor framework sets the stage for examining how the audit process unfolds once claims are selected for review.
Also Read: What are the Benefits and Types of Medical Coding Audits?
How Medicare Audits Work: Process, ADRs, and Appeals
Medicare audits follow a defined administrative structure, regardless of the contractor conducting the review. While the scope and intensity vary by audit type, the objective remains the same: determine whether submitted claims are supported by documentation and compliant with CMS coverage and billing rules.
What Triggers a Medicare Audit
Audits are typically initiated through data analysis, targeted review programs, or random selection. Common triggers include:
- High denial rates
- Billing patterns that differ from peer benchmarks
- Rapid growth in specific CPT or HCPCS codes
- Inconsistent documentation supporting medical necessity
- Unsupported diagnoses, including HCC conditions
- Improper modifier usage or unbundling
- Complaints or whistleblower reports
- Data anomalies identified through CMS analytics
CERT audits differ in that claims are selected through statistically valid random sampling rather than risk-based indicators.
The Audit Process Step by Step
Although timelines vary, most Medicare audits move through the following stages:
1. Claim Identification: A contractor selects claims for review based on analytics, targeted initiatives, or random sampling. At this stage, internal coordination is critical to define the scope and assign responsibility.
2. Additional Documentation Request (ADR): Providers receive a formal notice identifying the claims under review and outlining required documentation and deadlines.
Contractors commonly request:
- Complete medical records
- Physician orders and referrals
- Progress notes and operative reports
- Diagnostic test results
- Advance Beneficiary Notices (ABNs), when applicable
- Billing history and coding rationale
Failure to submit complete documentation within the specified timeframe generally results in denial.
3. Record Review and Determination: Auditors evaluate whether documentation supports:
- Medical necessity
- CPT and ICD-10 code selection
- Modifier usage
- Risk adjustment accuracy
- Compliance with LCD and NCD policies
Findings are issued in a written determination.
4. Demand Letter and Recoupment: If overpayments are identified, CMS issues a demand letter outlining repayment obligations. Recoupment may begin unless an appeal is filed within the allowed timeframe. In RAC and certain MAC audits, statistical sampling and extrapolation may extend repayment demands beyond the reviewed claims.
5. Appeals Process: Providers who dispute findings may proceed through multiple appeal levels:
- Redetermination
- Reconsideration
- Administrative Law Judge hearing
- Medicare Appeals Council review
Appeal outcomes depend on documentation integrity, accurate claim reconstruction, and defensible coding decisions.
The mechanics of review are structured and predictable. The financial and operational consequences depend on the strength of documentation, coding accuracy, and how efficiently the organization responds.
Also Read: Your 2026 Medical Coding Audit Checklist for Compliance & Clean Claims
Financial and Compliance Risks of Medicare Audits
Medicare audits extend beyond individual claim reviews. Depending on the findings, they can generate financial exposure, operational disruption, and increased regulatory oversight.
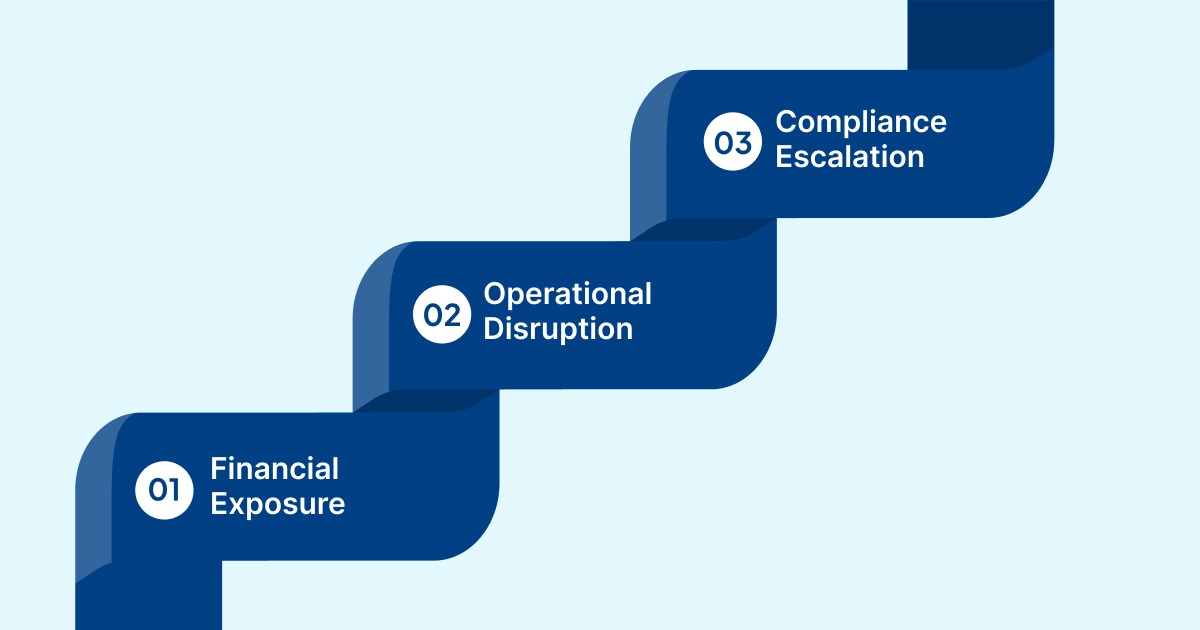
Financial Exposure
Audit findings may result in:
- Recoupment of identified overpayments
- Adjustments to future reimbursements
- Interest assessments on repayment amounts
- Administrative costs associated with appeals
When statistical sampling and extrapolation are applied, even modest documentation or coding error rates can translate into substantial repayment demands. In higher-risk reviews, such as UPIC investigations, payment suspension or enforcement action may follow.
Operational Disruption
Audit response requires coordination across coding, compliance, revenue cycle, clinical documentation, and IT teams.
Operational consequences often include:
- Coder time diverted from production
- Slower claim submission cycles
- Increased denial management workload
- Resource allocation to record retrieval and documentation assembly
Extended reviews or large documentation requests can materially slow routine revenue cycle activity.
Compliance Escalation
Uncorrected deficiencies increase the likelihood of intensified oversight. Escalation may include:
- Placement under pre-payment review
- Expanded claim sampling
- Broader investigative activity
- Referral to enforcement units
In many cases, repayment demands and regulatory scrutiny stem from recurring documentation and coding inconsistencies. Organizations that enforce disciplined documentation standards and continuous internal monitoring reduce both financial exposure and the risk of escalation.

Common Findings in Medicare Audits
Across all types of Medicare audits, findings typically stem from misalignment between clinical documentation, coding decisions, and claim submission. Most repayment demands trace back to preventable process gaps rather than isolated mistakes.
1. Documentation Issues
Medical records must clearly support the services billed and the level of care provided. Frequent deficiencies include:
- Incomplete or vague progress notes
- Missing or illegible provider signatures
- Unsupported or undocumented diagnoses
- Unclear admission status or level-of-care justification
- Missing required physician certifications
- Insufficient detail to establish the severity or intensity of services
- Improper post-denial documentation changes
When documentation does not substantiate medical necessity or code selection, denial or recoupment is likely.
2. Coding Issues
Incorrect code assignment can trigger audit findings even when services were appropriately delivered.
Common coding issues include:
- Upcoding E&M or procedure levels without supporting documentation
- Unbundling services that should be reported under a single comprehensive CPT code
- Improper modifier usage, including unsupported application of Modifier 25
- Lack of ICD-10 specificity
- Unsupported HCC condition capture
Coding must accurately reflect both the clinical encounter and CMS policy requirements. Variability creates data patterns that draw audit attention.
3. Billing Issues
Billing process weaknesses can also initiate a review. These often include:
- Duplicate claim submission
- Incorrect beneficiary information
- Billing that is inconsistent with actual service delivery
- Reporting service durations outside established norms
- Submitting claims that do not meet Medicare coverage criteria
- Failure to obtain a valid Advance Beneficiary Notice (ABN) when required
Audit findings typically reflect control failures rather than isolated mistakes. Organizations that enforce consistent documentation standards, coding validation, and billing oversight reduce downstream financial exposure.
How to Prepare for Medicare Audits
Audit readiness works best when it’s built into everyday operations. A structured, sequential approach improves clarity, accountability, and defensibility.
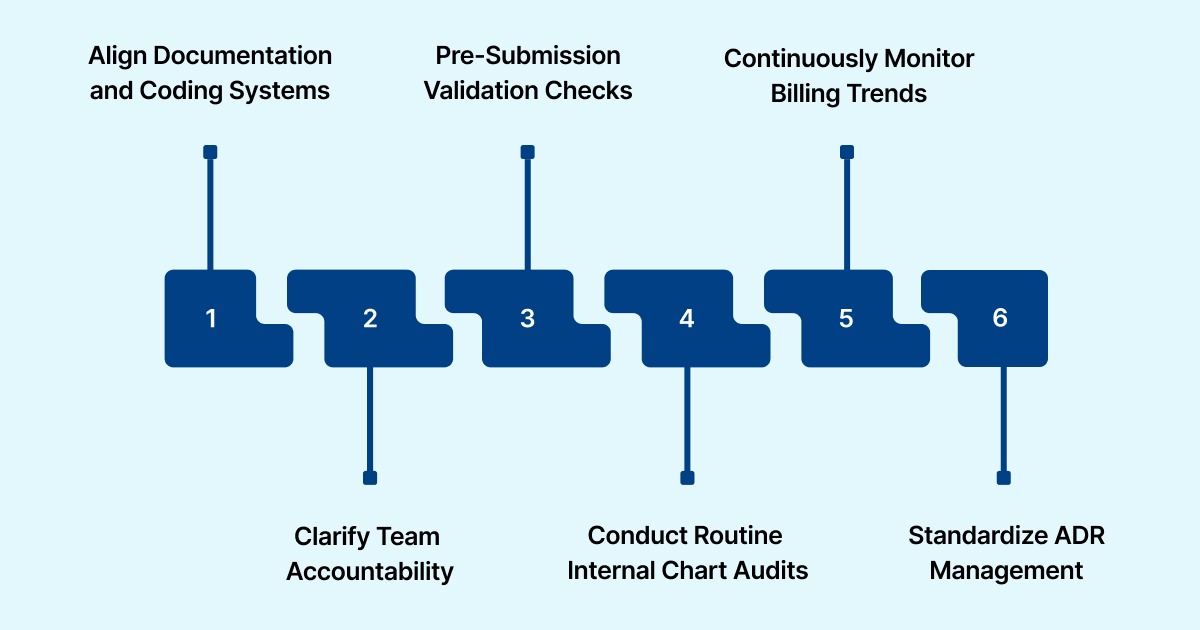
Step 1: Align Documentation and Coding Systems
Ensure clinical documentation directly supports CPT, ICD-10, HCPCS, and HCC code selection before claims are submitted. Tight alignment between EHR records and coding logic reduces discrepancies that often surface during audits.
Step 2: Assign Clear Accountability Across Teams
Define ownership for compliance oversight, coding quality review, ADR management, and escalation decisions. A clear role definition prevents delays, inconsistent communication, and fragmented responses during audit review.
Step 3: Implement Pre-Submission Validation Controls
Validate every claim for medical necessity support, modifier accuracy, NCCI compliance, and coverage alignment before submission. Early detection of documentation or coding gaps reduces denial rates and audit triggers.
Step 4: Conduct Routine Internal Chart Audits
Establish a structured internal review process to identify recurring coding errors, documentation deficiencies, and specialty-specific risk areas. Regular audits allow corrective action before external scrutiny occurs.
Step 5: Monitor Billing and Utilization Trends Continuously
Track outlier CPT usage, diagnosis distribution patterns, RAF score shifts, and denial categories. Data monitoring helps detect anomalies that could attract contractor review.
Step 6: Standardize ADR and Appeal Management
Create a centralized process for handling audit notices, including documentation tracking, quality review prior to submission, and structured appeal preparation. Organized, timely responses reduce financial exposure and strengthen defensibility.
As claim volumes increase and regulatory requirements evolve, maintaining consistency manually becomes more difficult.
How Automation Reduces Medicare Audit Risk
Audit risk increases when documentation, coding, and billing processes lack consistency. Manual workflows make it difficult to maintain uniform compliance at scale. Automation introduces structured validation that strengthens accuracy before claims reach Medicare review.
Automated systems support risk reduction by:
- Verifying that documentation supports medical necessity
- Ensuring CPT, ICD-10, and HCPCS codes align with clinical records
- Flagging unsupported modifiers or NCCI conflicts
- Identifying missing specificity or unsupported HCC conditions
- Detecting billing outliers through data analytics
These controls reduce technical errors that commonly trigger audits.
Automation also strengthens audit response. Time-stamped coding actions, version-controlled records, and organized documentation retrieval create clear audit trails. When an ADR arrives, structured data access reduces response time and improves appeal defensibility.
As audits become increasingly data-driven and regulatory expectations continue to shift, consistent validation at scale requires technology support. That is where RapidClaims fits into the revenue cycle.
How RapidClaims Strengthens Audit Readiness
RapidClaims is an AI-powered revenue cycle management platform designed to embed validation directly into everyday workflows. It combines advanced machine learning, natural language processing (NLP), and rule-based logic to automate key revenue cycle functions while preserving audit defensibility and oversight.
RapidCode – AI Medical Coding
- Automatically assigns CPT, ICD-10, and HCPCS codes based on clinical documentation
- Validates E&M levels and modifier usage
- Generates traceable audit logs for every coding decision
- Reduces variability and denial risk
RapidCDI – Clinical Documentation Integrity
- Identifies documentation gaps at the point of care
- Improves HCC condition capture and risk adjustment accuracy
- Ensures diagnoses are supported before claim submission
- Strengthens medical necessity documentation
RapidScrub – Pre-Submission Claim Validation
- Flags coding-documentation mismatches before submission
- Detects NCCI conflicts and coverage issues
- Improves first-pass claim acceptance rates
At scale, manual validation cannot keep up with growing claim volumes. RapidCode processes 1,000+ charts per minute and reduces denials by up to 70%, delivering measurable performance improvement without workflow disruption.

Conclusion
Types of medicare audits are built into the structure of federal reimbursement. The level of disruption they create depends on how consistently an organization manages documentation, coding, and billing before a review begins. Whether the audit is conducted by a RAC, MAC, CERT, UPIC, or OIG contractor, the standard remains the same: claims must be fully supported, accurately coded, and compliant with CMS policy.
Automation reinforces that discipline. Integrated validation, real-time documentation checks, and traceable audit logs improve accuracy while minimizing operational strain.
If your organization is evaluating ways to improve coding precision and strengthen audit readiness, explore how RapidClaims embeds AI-driven compliance controls directly into your revenue cycle workflows. Book your demo to see how RapidClaims strengthens coding accuracy and audit readiness across your revenue cycle.
FAQs
1. What is a Medicare audit?
A Medicare audit is a review of submitted claims to verify compliance with CMS coverage, coding, billing, and documentation requirements. Audits assess whether services were medically necessary and properly supported by the medical record.
2. What are the main types of Medicare audits providers face?
Common audit types include RAC, MAC medical reviews, CERT audits, UPIC investigations, SMRC reviews, and TPE audits. Each serves a different purpose, ranging from improper payment recovery to fraud investigation.
3. What is the difference between RAC and MAC reviews?
RAC audits focus on identifying improper payments after claims have been paid, often using data analytics and extrapolation. MAC reviews can occur pre- or post-payment and typically evaluate medical necessity and documentation compliance.
4. What typically triggers a Medicare audit?
Audits are commonly triggered by billing outliers, high denial rates, unsupported diagnoses, modifier misuse, or data anomalies compared to peer benchmarks. CERT audits may also select claims randomly.
5. How long do providers have to respond to an audit request or ADR?
Deadlines vary by contractor and audit type, but documentation is often required within 30 to 45 days. Providers must follow the exact timeline specified in the audit notice to avoid automatic denial.
6. Can small physician groups be audited?
Yes. Audit selection may be data-driven, complaint-based, or random. Organization size does not exempt providers from review.
7. Can automated coding reduce Medicare audit risk?
Yes. Automated coding tools help identify documentation gaps, coding inconsistencies, and unsupported diagnoses before submission. This reduces error rates and strengthens audit defensibility.
.png)
Mary Degapogu
Mary Degapogu is a proficient medical coder with 6 years of experience in E/M Outpatient and ED Profee coding, focused on precise code assignment and documentation compliance to drive clean claims and revenue integrity at RapidClaims.
Latest Post
expert insights with our carefully curated weekly updates
Related Post
Top Products

%201.png)
.jpg)
.jpg)






