AI In Medical Claims Processing Accuracy in 2026

Are your claims getting denied more than they should? For many providers today, a denial rate of 10% or higher has become the norm rather than the exception. This costs providers billions in delayed or lost revenue annually.
With payer policies growing more complex and claim volumes rising year over year, even a 2%–3% error rate can translate into millions of dollars of unrecovered cash. The administrative burden of correcting these errors falls on clinical and billing teams, pulling them away from patient care.
Which is why improving claims processing accuracy isn't just an operational goal anymore. It has become a financial survival strategy.
This blog will explore what claims processing accuracy really means, what's causing errors across the industry, and how AI and automation are helping providers get paid faster, cleaner, and more consistently.
At a Glance
- Claims processing accuracy determines whether providers get paid correctly on the first submission, reducing denials, delays, compliance risk, and rework costs.
- Most errors stem from coding mistakes, missing documentation, eligibility gaps, prior authorization failures, duplicate claims, and payer-specific rule mismatches.
- AI improves accuracy by automating coding, detecting documentation gaps, validating claims against live payer rules, scoring denial risk, optimizing HCC capture, and drafting appeals.
- Key KPIs to track include First-Pass Acceptance Rate (95%+ target), denial rate (<3% top performers), clean claim rate (98%+), A/R days (<40), coding accuracy (95%+), and cost to collect.
- RapidClaims delivers end-to-end automation, coding, CDI, scrubbing, and denial recovery, helping providers reduce denials, cut A/R days, and improve revenue within 30 days.
Table of Contents
- What is Claims Processing Accuracy?
- 6 Common Causes of Claim Processing Errors
- 8 Ways AI and Automation Improve Claims Processing Accuracy
- KPIs and Benchmarks to Measure Claims Processing Accuracy
- 5 Tips to Choose the Right Claims Processing Automation Solution
- Conclusion
- FAQs
What is Claims Processing Accuracy?
Claims processing accuracy refers to how consistently and correctly a healthcare claim moves from submission to reimbursement, without errors, rejections, or denials. It measures whether the right codes were applied, whether the claim matched payer requirements, and whether the provider got paid the correct amount the first time.
So, why does it matter?
- Revenue protection: Every inaccurate claim is either delayed, underpaid, or denied entirely, directly impacting cash flow.
- Compliance: Incorrect coding exposes providers to audits, penalties, and payer contract violations.
- Staff efficiency: Reworking denied claims consumes hours that clinical and billing teams could spend elsewhere.
- Patient trust: Billing errors that flow to patients create disputes, complaints, and damaged relationships.
When claims processing accuracy is high, providers get paid faster, with fewer follow-ups and less administrative overhead. When it's low, the ripple effects touch every corner of the revenue cycle. So, what's causing it to break down in the first place?
6 Common Causes of Claim Processing Errors
Most billing errors don't happen because teams aren't trying. They happen because the system is genuinely complex, and it's getting more complex every year. Payers update their rules constantly, coding guidelines shift, and patient records carry more data than ever. Here are the most common failure points:
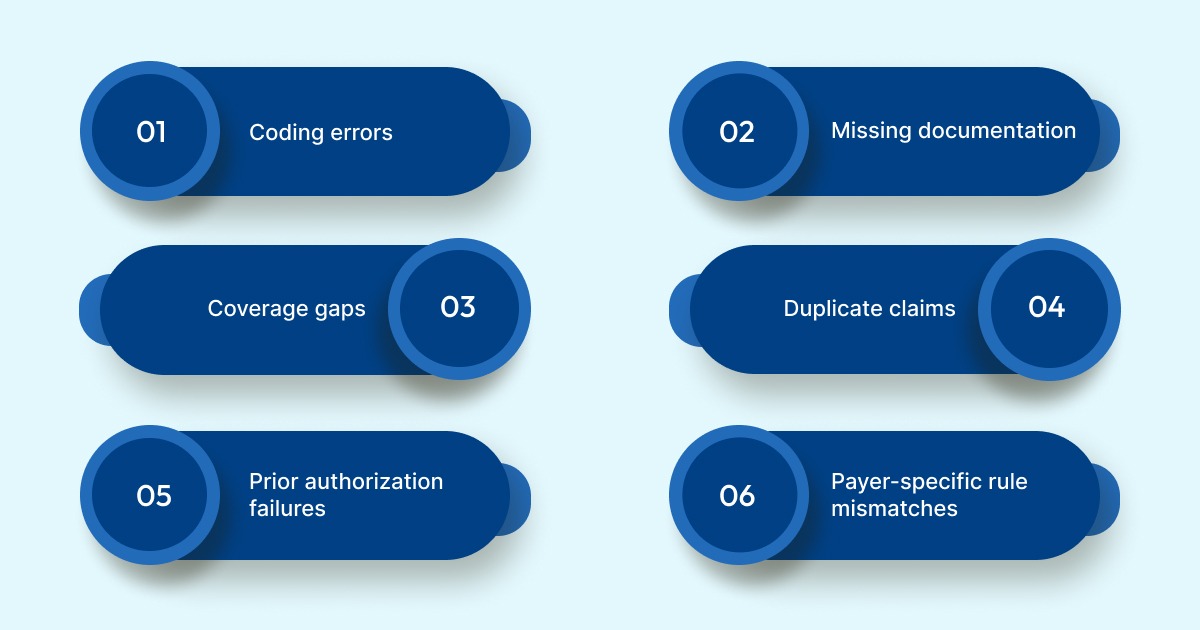
1. Coding errors: Incorrect, incomplete, or outdated ICD-10, CPT, or HCPCS codes are the single biggest driver of claim denials. A single digit off, or a code that doesn't match the documented diagnosis, is enough to trigger a rejection.
2. Missing or insufficient documentation: If a physician's note doesn't clearly support the diagnosis or procedure billed, payers will deny the claim, even if the care itself was appropriate and medically necessary.
3. Eligibility and coverage gaps: Submitting a claim for a patient whose coverage has lapsed, or for a service not covered under their specific plan, almost always results in a denial that could have been caught before submission.
4. Duplicate claims: Submitting the same claim more than once, whether by accident or system error, leads to automatic rejection and can flag a provider for audit.
5. Prior authorization failures: Many procedures require payer approval before the service is rendered. Skipping this step or not verifying that approval is current results in denials that are difficult to overturn after the fact.
6. Payer-specific rule mismatches: Each payer has its own billing requirements, edit rules, and contract terms. A claim that's perfectly valid for one payer may be denied by another for the exact same service.
These errors compound quickly. And when they pile up, the cost of rework often exceeds the value of the original claim. That's where AI and automation are changing the equation.
Also Read: RPA in Healthcare Claims Processing: Benefits and Use Cases
8 Ways AI and Automation Improve Claims Processing Accuracy
The traditional approach to claims accuracy. Manual review, rules-based scrubbers, and periodic audits were never designed for the volume and complexity providers face today. AI doesn't just speed things up. It addresses the root causes of errors in ways that static rules simply can't. Here's how:
1. Autonomous and Assisted Coding
AI systems like RapidCode™ can read clinical documentation and assign the correct ICD-10, CPT, and E&M codes automatically. Rather than a coder reviewing every chart from scratch, the AI generates a coded suggestion with line-level rationales.
So coders focus on review and exceptions instead of starting from zero. This alone can lift coder productivity and reduce cost-to-code significantly.
2. Real-Time Documentation Gap Detection
Before a claim is submitted, AI scans the underlying clinical notes for missing or insufficient documentation. If a diagnosis is coded but the physician's note doesn't clearly support it, the system flags it immediately. While the encounter is still fresh, corrections are easy to make.
3. Pre-Submission Claim Scrubbing
Instead of relying on static edit libraries that go stale quickly, AI-powered scrubbers like RapidScrub™ pull from continuously updated payer-specific edit rules. Every claim is validated against coverage, coding, and contract terms in under 200 milliseconds, catching issues before they reach the payer.
4. Eligibility Verification at Intake
AI integrates with payer APIs to confirm patient coverage in real time, before the appointment or at the point of billing. This eliminates an entire category of denials that stem from submitting claims for patients whose benefits have changed or lapsed.
5. Denial Probability Scoring
Not every claim needs the same level of human review. AI assigns a risk score to each claim based on historical denial patterns, payer behavior, and claim characteristics. High-risk claims get flagged for a second look. Clean claims move through automatically. This lets billing teams focus their attention where it actually matters.
6. HCC And Risk Adjustment Optimization
For providers operating in value-based care or Medicare Advantage, Hierarchical Condition Category (HCC) coding accuracy directly determines reimbursement. AI tools like RapidCDI™ analyze longitudinal patient records to surface HCC conditions that are clinically documented but not yet coded. This reduces missed revenue without creating compliance risk.
7. Automated Appeals Drafting
When denials do happen, AI can generate payer-specific appeal letters pre-populated with the relevant clinical documentation, coding rationale, and contract language. This cuts the appeal cycle time and removes the guesswork from recovery.
8. Continuous Learning From Payer Feedback
Every denial, every payer response, every policy update feeds back into the model. Unlike static rules engines that require manual updates, AI systems retrain on new data continuously. So accuracy improves over time rather than decaying as payer rules evolve.
Also Read: Guide to Automated Claims Processing in the Insurance Industry
The result is fewer denials, faster payments, and a billing team that spends less time firefighting and more time on complex cases. But to know whether it's working, you need to measure the right things.

KPIs and Benchmarks to Measure Claims Processing Accuracy
You can't improve what you don't measure. Most providers track denial rates, but that's only part of the picture. A complete view of claims processing accuracy requires a broader set of KPIs:
- First-Pass Acceptance Rate (FPAR): The percentage of claims accepted by the payer on the first submission. Industry benchmark is 95% or higher. Anything below 90% signals a systemic problem.
- Denial Rate: The percentage of submitted claims denied by the payer. The industry average hovers around 5%–10%, but top-performing revenue cycles stay under 3%.
- Clean Claim Rate: Claims submitted without errors that require no additional information or correction. A strong target is 98% or above.
- Days in Accounts Receivable (A/R): How long it takes to collect payment after a claim is submitted. Benchmark: under 40 days. High denial rates and rework cycles push this number up fast.
- Coding Accuracy Rate: The percentage of claims where codes are correct on the first pass, verified through internal audit or AI review. The target is more than 95%.
- Denial Overturn Rate: Of the claims you appeal, what percentage do you win back? A healthy rate is 60%–70% or higher.
- Cost to Collect: The total administrative expense incurred to collect one dollar of revenue. Automation directly reduces this metric.
Also Read: Average Claim Denial Rate in 2025: Benchmarks and Key Drivers
Tracking these KPIs together gives you a full picture of where accuracy is breaking down and where the biggest recovery opportunity lies. Once you know where you stand, the next step is choosing the right tools to close the gap.
5 Tips to Choose the Right Claims Processing Automation Solution
There's no shortage of vendors claiming to solve the accuracy problem. The differences between them matter more than the marketing suggests. Here's what to actually evaluate:
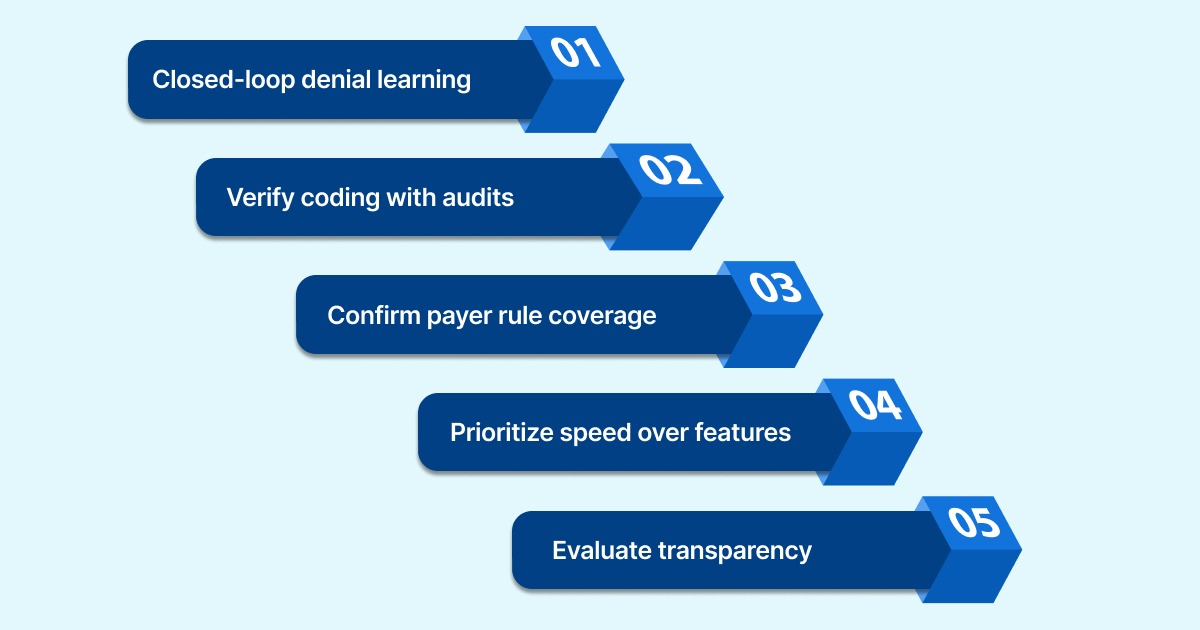
1. Prioritize deployment speed over feature volume: A solution that takes 6 months to implement gives you nothing for 6 months. Look for platforms that can go live with a small data set and start generating ROI faster. Implementation complexity is often where ROI projections fall apart.
2. Verify coding accuracy with audited data, not marketing claims: Any vendor can publish an accuracy percentage. Ask how it was measured, by whom, and across what specialties. Audited accuracy on your own chart mix, not a curated benchmark set, is the only number that matters for your organization.
3. Confirm payer rule coverage and update frequency: A scrubber is only as good as its edit library. Ask vendors how frequently payer rules are updated, whether updates are manual or automated, and whether the system covers your specific payer mix. A tool trained on national averages may miss region-specific or plan-specific rules that affect your claims daily.
4. Look for closed-loop learning between denial recovery and claim submission: The best systems feed denial outcomes back into the coding and scrubbing layers. If a payer denies a claim for a specific reason, that pattern should automatically update future edits. Without this loop, you're fixing the same errors repeatedly.
5. Evaluate transparency and audit trail capability: Especially in coding, you need to know why a code was assigned. Look for systems that provide line-level rationales tied to specific documentation, not black-box outputs. This matters for compliance, for coder training, and for defending claims in audits.
Also Read: Challenges and Strategies in Health Insurance Claims Processing
Choosing the right solution isn't about finding the most sophisticated AI. It's about finding a system that fits your workflow, covers your payer mix, and improves measurably within a defined timeframe. RapidClaims is built exactly with that in mind.

How RapidClaims Addresses Claims Processing Accuracy End-to-End
Providers today are dealing with a compounding problem: coding errors, missed HCC conditions, payer-specific denials, and a recovery backlog that keeps growing. Each one of these issues requires a different fix, and most point solutions only address one piece of the puzzle.
RapidClaims is an AI-powered revenue cycle platform that covers the full claim lifecycle, from coding and documentation integrity to pre-submission scrubbing and denial recovery, in a single integrated system.
- RapidCode™ assigns ICD-10, CPT, and E&M codes autonomously, processing 1,000+ charts per minute at 96%+ audited accuracy across 36+ specialties
- RapidCDI™ surfaces missed HCC conditions and RAF opportunities at the point of care, with a 25% average RAF accuracy lift and $2.2M in documented annual revenue gains
- RapidScrub™ validates every claim against 119M smart edits before submission, reducing denials by 70% and cutting A/R days by 5
- RapidRecovery™ manages denial overturn with AI-drafted appeals and a success-based model — providers pay only on dollars recovered
- Full audit trails, AHIMA-compliant documentation, and continuous learning from payer responses are built into every module
RapidClaims deploys in under 30 days with as few as 500 historical charts, integrating directly with Epic, Cerner, Athena, and major clearinghouses via SMART-on-FHIR and X12 837.
Conclusion
Claims processing accuracy in 2026 depends on the efficiency of your system workflow. Manual coding, static scrubbers, and reactive denial management were never built to handle the volume and complexity that providers face today. The providers seeing the strongest financial outcomes are those who have replaced reactive workflows with AI systems that catch errors before they become denials, and recover revenue faster when they do.
RapidClaims gives providers a cost-effective path to fixing this end-to-end, from the first line of a clinical note to the final dollar recovered on a denied claim. With proven results across physician groups, FQHCs, and ACOs, it's a platform built to deliver measurable ROI within 30 days.
Ready to see what your denial rate should actually look like? Request a personalized demo to run an ROI estimate on your own chart data.
FAQs
1. What's the difference between a claim rejection and a claim denial?
A rejection happens before the claim is processed. It's returned because of a technical error, such as a missing field or invalid code format. A denial happens after processing, meaning the payer reviewed the claim and decided not to pay. Rejections are usually easier to fix; denials often require an appeal with supporting documentation.
2. How does prior authorization affect claims processing accuracy?
Prior authorization failures are one of the top denial drivers. If a service requires payer approval before it's rendered and that approval isn't obtained, or isn't correctly documented on the claim, the payer will deny it regardless of medical necessity. Automated eligibility and PA verification at the scheduling or intake stage eliminates most of these.
3. Can small or independent practices benefit from AI-powered claims automation, or is it only for large health systems?
AI coding and scrubbing tools are increasingly designed to scale down as well as up. Platforms like RapidClaims can go live with as few as 500 charts, making them viable for smaller physician groups, specialty practices, and independent billing companies — not just enterprise health systems.
4. What happens to claims accuracy when a practice adds a new specialty or expands its payer contracts?
New specialties bring new coding guidelines, and new payer contracts bring new billing rules. Both create a temporary spike in denial rates if the team isn't trained and systems aren't updated. AI platforms that continuously learn from payer responses and cover a broad specialty range handle this transition better than static rules engines.
5. How often do payer rules change, and how does that affect accuracy over time?
Payer rules change constantly. CMS updates quarterly, commercial payers update their edit libraries on rolling schedules, and LCD/NCD policies shift based on clinical evidence. A claims scrubber that isn't updated in real time becomes less accurate over time. AI-powered systems that pull from live payer bulletins and retrain on denial data maintain accuracy as the rules evolve.

Rejones Patta
Rejones Patta is a knowledgeable medical coder with 4 years of experience in E/M Outpatient and ED Facility coding, committed to accurate charge capture, compliance adherence, and improved reimbursement efficiency at RapidClaims.
Latest Post
expert insights with our carefully curated weekly updates
Related Post
Top Products

%201.png)