Top Benefits of Process Automation in Healthcare

Revenue cycle pressure is accelerating. According to Experian Health’s 2025 State of Claims survey, 41% of providers report denial rates of 10% or higher, and more than half say submitting clean claims is harder than it was a year ago. That means a significant share of claims require rework, appeals, or write-offs, slowing cash flow and increasing administrative cost.
Manual coding reviews and reactive denial management cannot keep up with expanding payer scrutiny, HCC model updates, and growing documentation complexity. Business process automation shifts revenue cycle teams from fixing errors after submission to preventing them before claims are sent out.
By validating documentation early, enforcing payer rules consistently, and standardizing coding decisions, automation reduces denial risk at scale. In this article, we examine how automation strengthens coding accuracy, improves claim performance, and brings greater stability to the revenue cycle.
TL;DR
- Denial pressure is rising. Manual workflows can’t keep pace with payer complexity, HCC updates, and documentation demands, leading to rework, delayed cash flow, and higher administrative costs.
- The benefits of process automation delivers are measurable. Organizations see fewer denials, higher first-pass yield, improved coding accuracy, and stronger RAF capture.
- Modern automation goes beyond RPA. AI-driven systems interpret clinical documentation, enforce payer rules early, and maintain audit-ready decision trails.
- When implemented strategically, automation stabilizes revenue performance. It reduces operational risk, improves throughput, and allows coding teams to focus on higher-value work.
Table of Contents
- How Legacy Revenue Cycle Workflows Increase Denials and Cost?
- What is Process Automation in Healthcare?
- Why Basic RPA Is Not Enough for Revenue Cycle Management
- How Process Automation Works in Healthcare Revenue Cycle
- Top Benefits of Process Automation in Healthcare Operations
- Real-World Use Cases of Automation in Healthcare Organizations
- Best Practices for Revenue Cycle Automation
- Common Automation Pitfalls in Healthcare Revenue Cycle
- RapidClaims: A Purpose-Built Platform for Revenue Cycle Automation
- Conclusion
- FAQs
How Legacy Revenue Cycle Workflows Increase Denials and Costs
Manual workflows remain common across revenue cycle operations. Charts are reviewed one by one, codes are validated manually, and claims are scrubbed using static rules that lack clinical context. While familiar, these processes create consistent points of failure.
Common breakdowns include:
- Data entry errors that result in coding mismatches
- Incomplete documentation that leads to denials
- Routine exceptions routed unnecessarily to senior staff
- Payer rules applied late in the submission cycle
The impact is measurable and financial:
- Higher denial rates
- Lower first-pass yield
- Longer days in accounts receivable
- Increased cost per denied claim
At the same time, CMS requirements and HCC model transitions such as V24 to V28 continue to add regulatory complexity. As documentation volume increases, manual processes struggle to maintain accuracy and speed.
Under these conditions, the benefits of process automation become operationally critical. Automation does not simply accelerate tasks, it applies payer logic earlier, reduces preventable errors, and stabilizes revenue performance.
If manual processes are the root of denial risk and cost escalation, the next question is clear: what does a modern alternative actually look like?
What is Process Automation in Healthcare?
Process automation in healthcare refers to intelligent systems that standardize, execute, and monitor workflows across revenue cycle operations.
Within revenue cycle management, automation supports:
- Clinical documentation intake
- Code abstraction and validation
- Pre-submission claim scrubbing
- Denial identification and routing
- Audit logging and compliance reporting
Unlike basic rule-based RPA, modern automation applies natural language processing and machine learning to interpret unstructured clinical documentation. It detects coding gaps, evaluates payer-specific requirements, and applies logic dynamically instead of relying only on static rules.
The result is not just faster task execution, but informed decision support across coding and claims workflows.
However, not all automation operates at this level. Many organizations find that simple task scripting alone does not resolve the complexity of modern revenue cycle operations.
Why Basic RPA Is Not Enough for Revenue Cycle Management
Revenue cycle operations depend on clinical interpretation, payer-specific logic, and regulatory alignment. Basic robotic process automation (RPA) was built for repetitive digital tasks, not for managing the variability and compliance demands of modern claims workflows.

a) RPA Handles Repetition, Not Clinical Judgment
RPA works well in predictable environments. It can:
- Move data between systems
- Populate predefined fields
- Trigger routine workflow steps
But coding and claims processing require interpretation. Clinical notes often contain nuance, incomplete details, or context that static rules cannot evaluate accurately.
b) Claims Workflows Are Exception-Driven
Revenue cycle processes rarely follow a fixed path. Automation breaks down when it encounters:
- Ambiguous or incomplete documentation
- Complex CPT or HCPCS combinations
- HCC logic tied to CMS updates such as V24 to V28
- Medical necessity documentation gaps
Static rule sets cannot adapt dynamically to these variations without constant manual correction.
c) Fragmented Systems Reduce Automation Accuracy
Revenue cycle operations span multiple systems, including:
- EHR platforms
- Clearinghouses
- Claim scrubbers
- Risk adjustment tools
- Compliance systems
Without normalized data and structured HL7 or FHIR integrations, automation produces inconsistent outputs or shifts exceptions back to manual review.
d) Compliance Requires Traceable Decision Logic
Automation that influences coding must:
- Align with ICD-10 and CPT standards
- Reflect CMS documentation policies
- Apply payer-specific LCD and NCD edits
It must also maintain clear audit trails, documented code rationale, and logged override history. Tools that cannot explain their recommendations increase audit exposure rather than reducing it.
e) Scalable Automation Requires Integrated Intelligence
As chart volumes increase and payer rules evolve, revenue cycle teams need systems that combine:
- Clinical interpretation
- Dynamic payer rule application
- Secure system integration
- Structured exception routing
RPA automates tasks. Modern revenue cycle automation must support informed decision-making. Addressing these gaps requires a more integrated approach, one that combines clinical interpretation, payer logic, and workflow orchestration.
How Process Automation Works in Healthcare Revenue Cycle
Effective revenue cycle automation relies on integrated components that operate across clinical and billing systems. Each layer supports a specific function in the coding-to-claim lifecycle.
1. Data Ingestion and Normalization: Automation begins by securely extracting structured and unstructured data from EHR systems, including clinical notes, orders, and problem lists. This information is standardized into consistent formats so downstream models can process it reliably.
2. Coding Intelligence Layer: A coding engine uses natural language processing and clinical context models to analyze documentation and generate ICD-10, CPT, or HCC code suggestions. Each recommendation is linked to supporting documentation and logged for audit traceability.
3. Payer Rules and Validation Engine: Before submission, claims are evaluated against payer-specific edits, coverage policies, and documentation requirements. Real-time validation identifies coding conflicts, missing elements, and compliance gaps early in the workflow, reducing preventable rejections.
4. Exception Management and Workflow Routing: Automation does not eliminate oversight. Routine cases move forward automatically, while ambiguous or high-risk claims are routed to coders or auditors for review. This approach maintains quality control while improving throughput.
5. EHR and System Integration: Automation must integrate seamlessly with existing infrastructure. HL7 and FHIR-based connectivity enables secure data exchange between the automation platform, EHR systems, clearinghouses, and billing tools without disrupting operational workflows.
These technical capabilities are important, but their real value becomes evident when applied directly to coding and claims workflows.

Top Benefits of Process Automation in Healthcare Operations
When deployed across revenue cycle workflows, the benefits process automation delivers are operational and financial. Automation strengthens coding accuracy, reduces preventable denials, and improves cash flow stability without increasing staffing pressure.
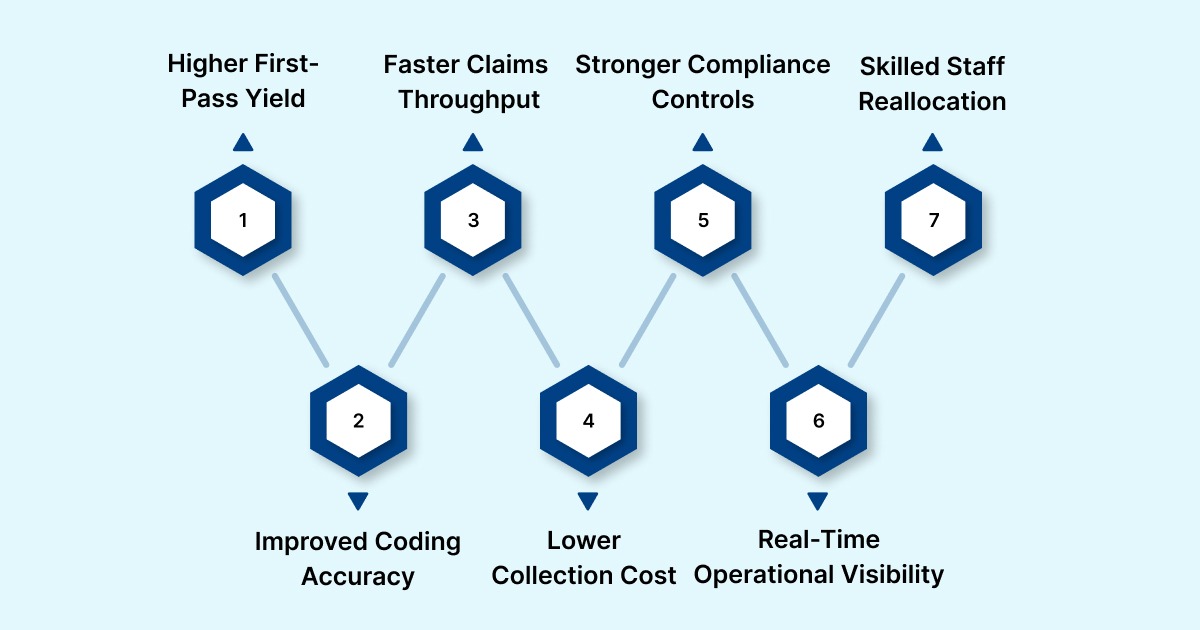
1. Fewer Denials and Higher First-Pass Yield
Automation applies payer logic and documentation checks before submission, reducing avoidable rejection triggers.
It improves performance by:
- Validating claims against CMS guidelines and NCCI edits prior to submission
- Detecting missing documentation that could cause medical necessity denials
- Identifying invalid CPT or HCPCS combinations early
- Applying payer-specific coverage policies systematically
Instead of correcting errors after adjudication, teams prevent them at the source.
2. Improved Coding Accuracy and Stronger RAF Capture
Natural language processing reviews structured and unstructured documentation to ensure coding reflects supported clinical evidence.
Automation enhances accuracy by:
- Extracting diagnoses directly from clinical notes
- Linking suggested ICD-10, CPT, and HCC codes to source documentation
- Flagging unsupported or vague diagnoses
- Identifying chronic conditions relevant for risk adjustment
In value-based and Medicare Advantage contracts, consistent HCC capture directly influences RAF scoring and defensible reimbursement.
3. Faster Claims Throughput and Shorter A/R Cycles
Automation reduces friction across the coding-to-submission workflow.
It accelerates processing by:
- Standardizing chart review steps
- Applying validation checks earlier in the workflow
- Routing routine claims automatically
- Escalating only high-risk or ambiguous cases
This shortens submission timelines and supports more predictable reimbursement cycles.
4. Lower Cost to Collect Without Expanding Headcount
Automation reduces manual workload while preserving professional oversight.
It improves cost efficiency by:
- Eliminating repetitive data abstraction tasks
- Reducing duplicate documentation review
- Minimizing rework from preventable denials
- Allowing systems to absorb increased chart volume
As volumes grow, automation scales without requiring proportional increases in staffing.
5. Stronger Compliance Controls and Audit Readiness
Revenue cycle automation must support defensibility, not just efficiency.
It strengthens compliance by:
- Logging detailed audit trails for coding decisions
- Recording override rationale and user activity
- Enforcing documentation completeness requirements
- Maintaining alignment with ICD-10, CPT, and CMS standards
During CMS reviews or payer audits, structured documentation trails reduce exposure and response time.
6. Real-Time Operational Visibility
Automation provides structured insight into workflow performance.
Leaders gain visibility through:
- Early detection of denial patterns
- Identification of recurring coding discrepancies
- Monitoring of backlog and exception volume
- Tracking documentation gaps before submission
This allows proactive correction instead of post-payment recovery efforts.
7. Reallocation of Skilled Staff to Higher-Value Work
Automation shifts repetitive tasks away from experienced professionals.
This enables teams to focus on:
- Complex cases requiring clinical judgment
- Appeals and denial prevention strategies
- Documentation improvement initiatives
- Quality assurance and compliance oversight
Rather than replacing coders, automation increases the strategic value of their expertise.
Together, these outcomes demonstrate that process automation is not limited to efficiency gains. It strengthens financial predictability, reduces operational risk, and supports sustainable revenue cycle performance.
Real-World Use Cases of Automation in Healthcare Organizations
Process automation delivers measurable results across different healthcare settings. While operational pressures vary, the impact consistently centers on denial reduction, coding consistency, and revenue predictability.
Large Health Systems
Health systems manage high inpatient and outpatient volumes across multiple departments. Variations in documentation quality and coding practices often lead to inconsistent claim outcomes.
Automation improves control by:
- Standardizing coding logic across facilities
- Detecting documentation gaps before submission
- Centralizing compliance tracking
In inpatient-focused deployments, health systems have reduced coding-related denials within the first quarter while increasing coder throughput and reducing rework.
Physician Groups
Physician groups, particularly those participating in Medicare Advantage contracts, must meet increasing documentation standards without proportional staffing growth.
Automation supports scalability by:
- Extracting supported diagnoses directly from clinical notes
- Flagging documentation gaps that affect risk adjustment
- Reducing post-bill corrections and clarification cycles
Groups implementing AI-assisted coding have increased charts processed per coder while improving coding consistency.
Medical Billing Companies
Billing organizations working across multiple clients must enforce varied payer rules while maintaining quality assurance.
Automation enables them to:
- Apply payer-specific edits consistently
- Validate documentation prior to submission
- Route complex exceptions efficiently
Firms using automated validation have reduced common rejection causes and improved overall claim throughput without compromising compliance oversight.
Across these settings, the benefits process automation translates into more predictable revenue performance, lower denial exposure, and stronger audit readiness. Achieving similar results requires a structured and disciplined implementation approach.
Best Practices for Revenue Cycle Automation
Automation produces measurable results when deployed with clear scope, defined accountability, and disciplined execution. A structured rollout reduces operational disruption and improves long-term sustainability.
1. Prioritize High-Impact Workflows: Begin deployment in areas with the highest financial exposure, such as high-volume specialties, claim categories with recurring denials, and risk-adjusted populations like Medicare Advantage. Targeting these workflows first allows organizations to demonstrate measurable improvements before expanding automation more broadly.
2. Define Baselines Before Implementation: Establish current performance levels to measure impact accurately. Baseline metrics should include denial rates, A/R days, coding turnaround time, RAF capture, and coder productivity. Regular review intervals ensure performance gains are validated and sustained.
3. Implement Through a Controlled Pilot: Deploy automation within a defined scope, such as a specific specialty or claim type, with clear success criteria. Early coordination between revenue cycle leadership, IT, compliance, and coding teams prevents workflow fragmentation. A pilot phase enables process refinement before scaling.
4. Integrate Securely With Core Systems: Automation must align with existing infrastructure, including EHR platforms, clearinghouses, and payer rule databases. Secure HL7 or FHIR-based integrations and role-based access controls protect data integrity and regulatory compliance.
5. Preserve Human Oversight: Automation supports efficiency but does not eliminate professional review. Define thresholds for manual intervention, establish quality assurance checkpoints, and maintain escalation pathways for complex cases. Governance safeguards both coding accuracy and compliance integrity.
6. Optimize Continuously: Revenue cycle rules and documentation standards evolve. Automation must be monitored, updated, and recalibrated to reflect payer changes, regulatory updates, and shifting documentation patterns. Automation in revenue cycle operations is an ongoing capability, not a one-time deployment.
Even with structured implementation, risks remain if governance and data quality are not maintained.

Common Automation Pitfalls in Healthcare Revenue Cycle
Automation delivers results only when governance, data integrity, and team alignment are maintained. Without these controls, implementation risks increase.
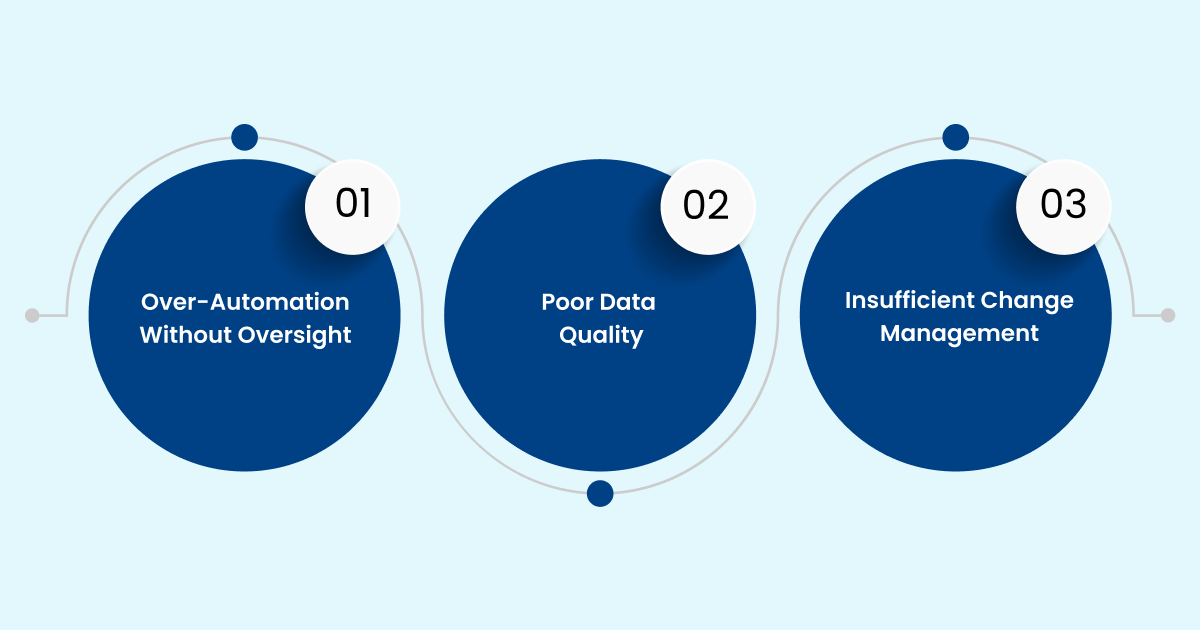
- Over-Automation Without Oversight: Fully automating workflows without defined exception thresholds can introduce systematic errors at scale. Clear review checkpoints and escalation protocols are necessary to preserve coding accuracy and compliance integrity.
- Poor Data Quality: Automation depends on reliable inputs. Incomplete, inconsistent, or poorly structured EHR data reduces model accuracy and increases manual correction. Ongoing data hygiene and documentation standards remain essential.
- Insufficient Change Management: Successful adoption requires transparency and training. Medical coders and revenue cycle staff must understand how AI-generated suggestions are derived and when to intervene. Without engagement and education, resistance and underutilization can undermine results.
Addressing modern revenue cycle challenges therefore requires more than generic automation tools. Effective solutions must combine clinical context, dynamic payer rule enforcement, structured governance, and smooth system integration.
RapidClaims: A Purpose-Built Platform for Revenue Cycle Automation
Healthcare revenue cycle complexity demands automation designed specifically for coding and claims workflows. RapidClaims is an AI-powered revenue cycle management platform built to reduce preventable denials, strengthen coding accuracy, and improve reimbursement predictability while maintaining professional oversight.
RapidClaims includes three core products that work together to optimize revenue cycle performance:
- RapidCode – Autonomous medical coding that uses AI to assign ICD-10, CPT, and HCC codes with audit-ready evidence, supporting high coding accuracy across specialties.
- RapidScrub – Proactive denials prevention that evaluates claims against payer-specific rules, CMS guidelines, and compliance standards before submission, reducing rejection risk.
- RapidCDI – Documentation and risk intelligence that enhances clinical documentation, improves HCC capture, and supports risk adjustment workflows for more accurate reimbursement.
Together, these capabilities combine coding intelligence, payer rule validation, and structured workflow orchestration. The result is scalable automation that improves denial control, coding consistency, and compliance readiness without sacrificing human oversight.

Conclusion
Manual revenue cycle workflows increase denial risk, prolong days in accounts receivable, and divert skilled coding teams toward repetitive correction work. As payer requirements tighten and documentation standards evolve, these inefficiencies directly impact cash flow, margin stability, and compliance exposure.
The benefits of process automation delivers are measurable and strategic. Organizations gain higher coding accuracy, stronger RAF capture, improved first-pass yield, and reduced preventable denials. When implemented with proper governance and human oversight, automation transforms revenue cycle operations from reactive recovery to proactive control.
Book a demo to see how RapidCode, RapidScrub, and RapidCDI can reduce preventable denials, improve coding accuracy, and shorten days in A/R.
FAQs
1. How does process automation reduce claim denials?
Automation applies payer-specific rules and documentation checks before claims are submitted. By identifying mismatches and missing information early, it reduces preventable rejections and improves first-pass approval rates.
2. Will automation replace medical coders?
No. Automation handles routine abstraction and validation tasks, while coders review exceptions and complex cases. It increases productivity without removing professional oversight.
3. How quickly can organizations see results after implementation?
Most teams observe measurable improvements in denial rates and throughput within 8–12 weeks, depending on workflow scope and integration readiness.
4. Can automation integrate with existing EHR systems?
Yes. Modern platforms use standards such as HL7 and FHIR to connect with EHRs, clearinghouses, and billing systems while maintaining secure data exchange.
5. Is AI-assisted coding audit-ready?
When implemented correctly, automation logs code rationale, tracks overrides, and maintains documentation trails. This supports compliance reviews and external audits.
.png)
Ayeesha Siddiqua
Ayeesha Siddiqua is a highly experienced medical coding professional with 22 years of expertise in E/M Outpatient, Radiology, and Interventional Radiology (IVR), ensuring coding accuracy, regulatory compliance, and optimized reimbursements at RapidClaims.
Latest Post
expert insights with our carefully curated weekly updates
Related Post
Top Products

%201.png)