Medical Assistant vs Medical Billing and Coding: Key Differences Explained

Modern healthcare organizations are under constant pressure. Documentation gaps rarely remain invisible. They surface as denied claims, delayed reimbursements, and increased audit exposure.
According to the American Hospital Association, hospitals spend nearly $20 billion annually managing billing and insurance complexity. A significant portion of that cost stems from documentation errors, coding inconsistencies, and workflow breakdowns between clinical and revenue teams.
This is why the medical assistant vs medical billing and coding comparison is not simply a staffing discussion. It is a revenue integrity decision.
Medical assistants shape documentation at the point of care. Coding professionals determine how that documentation is translated into compliant, reimbursable claims. When the transition between these roles weakens, financial performance follows.
This article examines both roles through an operational lens and outlines how stronger workflow alignment and automation can protect margins and reduce denial risk.
TL;DR
- Medical assistants support clinical workflows, ensuring accurate documentation and smooth patient flow, but they do not manage coding or claims.
- Medical billing and coding professionals directly impact revenue, translating documentation into compliant claims that determine denial rates and reimbursement speed.
- Revenue performance depends on the handoff between documentation and coding. Misalignment increases denials, delays payments, and raises audit risk.
- AI-powered coding automation strengthens this transition, improving accuracy, reducing rework, and enabling scalable revenue cycle operations without proportional staffing growth.
Table of Contents
- What Does a Medical Assistant Do?
- What Does a Medical Coding and Billing Specialist Do?
- Medical Assistant vs Medical Billing and Coding: Key Differences
- Similarities Between Medical Assistants and Medical Coding Professionals
- Operational Impact on Revenue Cycle Performance
- When Should You Expand Medical Assistant vs Coding Capacity?
- Where AI-Powered Medical Coding Automation Creates Leverage
- Medical Assistant vs Medical Billing and Coding: Compensation and Market Demand
- RapidClaims: AI-Powered Medical Coding Automation
- Conclusion
- FAQs
What Does a Medical Assistant Do?
Medical assistants support clinical care and front-office workflows. Their primary responsibility is to ensure accurate documentation and efficient patient flow during each encounter.
Core responsibilities include:
- Recording vital signs and updating medical histories
- Preparing patients and exam rooms
- Assisting physicians during examinations and procedures
- Administering injections and collecting specimens, where permitted
- Performing routine diagnostic tests
- Updating information within the EHR
- Coordinating scheduling and front-desk activities
They also reinforce care instructions, maintain infection control standards, and support urgent clinical needs when required. From an operational standpoint, medical assistants influence documentation completeness and throughput. They do not assign diagnosis or procedure codes, but the accuracy of the information they record directly affects downstream coding, billing, and compliance.
Most medical assistants work in physicians' offices, outpatient clinics, and specialty practices. The role is hands-on, fast-paced, and closely integrated with clinical teams.
While medical assistants shape documentation at the point of care, the financial outcome depends on how that documentation is interpreted and coded. That responsibility rests with coding and billing professionals.
What Does a Medical Coding and Billing Specialist Do?
Medical coding and billing specialists manage the financial translation of clinical care. Their responsibility is to convert provider documentation into accurate, compliant claims that can be reimbursed.
Core responsibilities include:
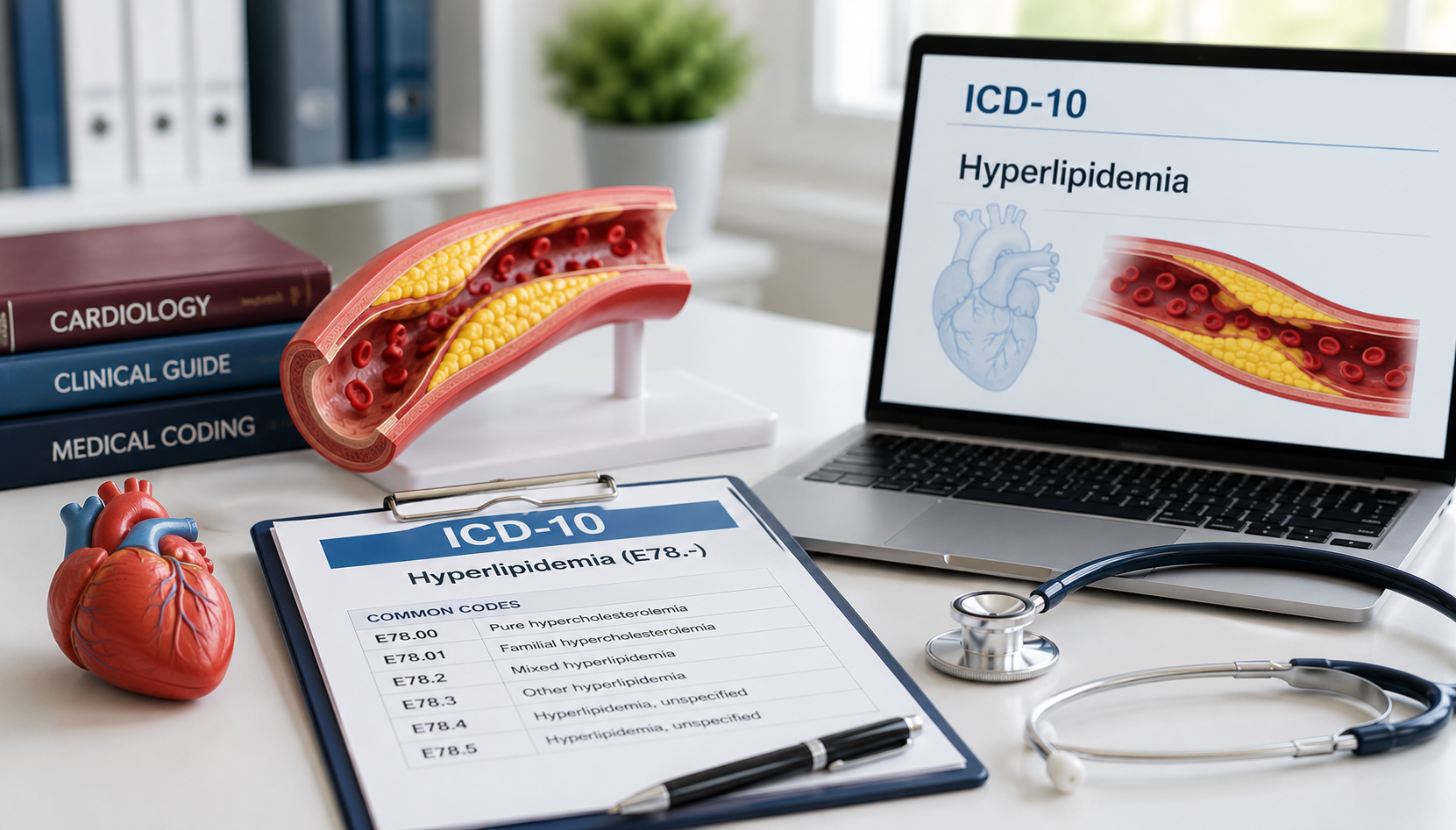
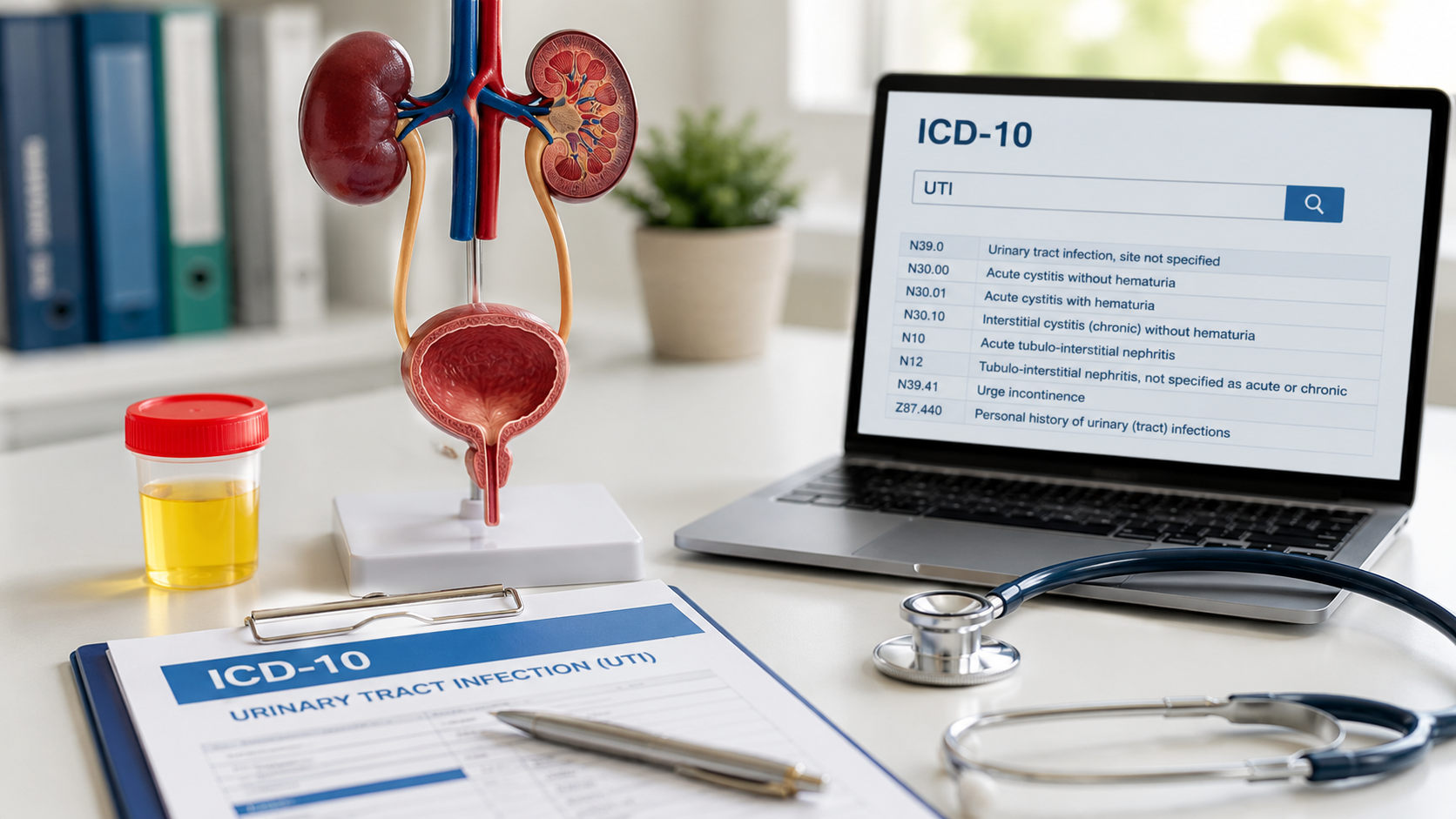
- Assigning ICD-10, CPT, and HCPCS codes
- Validating documentation against CMS and payer guidelines
- Preparing and submitting claims
- Monitoring claim status and posting payments
- Reconciling remittance advice
- Investigating denials and managing appeals
- Supporting audits and compliance reviews
- Coordinating required pre-authorizations
This role directly affects claim accuracy, reimbursement timelines, denial rates, and audit exposure. Small coding inconsistencies can result in payment delays or compliance findings.
Coding and billing professionals work in physician practices, hospitals, specialty clinics, and billing organizations. Because the work is documentation-driven, it often follows structured workflows and supports remote or hybrid models.
Formal coding education and certification are typically required due to regulatory complexity and payer requirements.
Also Read: Becoming a Medical Coding and Billing Specialist: Steps to Get Certified
Now that both roles are clearly defined, the distinction becomes easier to evaluate. The differences are not subtle, and they carry measurable revenue implications.
Medical Assistant vs Medical Billing and Coding: Key Differences
Medical assistants and medical billing and coding professionals both contribute to healthcare delivery, but they operate in different phases of the workflow. One focuses on clinical execution. The other manages revenue cycle integrity.
Below is a structured comparison:
Role Focus and Primary Work
- Medical assistants provide clinical support and office coordination. Their primary work includes patient intake, recording vital signs, preparing exam rooms, assisting physicians, and managing scheduling. They ensure patient visits run efficiently and that documentation is captured accurately in the EHR.
- Medical billing and coding professionals manage revenue cycle execution. Their primary work involves translating clinical documentation into standardized codes, submitting claims, managing denials, and validating compliance with payer and CMS guidelines.
Revenue Cycle Impact
- Medical assistants influence revenue indirectly. The quality of the documentation they record affects coding accuracy, but they do not assign diagnosis or procedure codes.
- Medical billing and coding professionals have a direct revenue impact. Their coding decisions determine claim acceptance, reimbursement timelines, denial rates, and audit exposure.
Training and Qualifications
- Medical assistants typically enter the field through certificate programs or on-the-job training, with certification often preferred by employers. Training focuses on clinical procedures and administrative coordination.
- Medical billing and coding professionals require formal coding education. Most employers expect a certificate or associate degree along with industry-recognized credentials. Training centers on ICD-10, CPT, HCPCS, and payer compliance frameworks.
Work Environment and Structure
- Medical assistants work primarily in physician offices, outpatient clinics, and urgent care centers. The role is on-site, patient-facing, and fast-paced.
- Medical billing and coding professionals work in structured, documentation-driven environments within physician groups, hospitals, and billing organizations. Because the work is system-based, it often supports remote or hybrid models.
Industry Demand Drivers
- Demand for medical assistants is largely driven by outpatient growth and expanding access to care.
- Demand for medical billing and coding professionals is driven by increasing regulatory complexity, value-based care requirements, and payer scrutiny.
Despite structural differences, both roles share foundational competencies that support healthcare delivery.
Similarities Between Medical Assistants and Medical Coding Professionals
While medical assistants and medical coding professionals perform different functions, both require core competencies that support accurate, compliant healthcare operations.
1. Foundational Healthcare Knowledge
Both roles depend on a working understanding of medical terminology, common procedures, and clinical documentation standards. This shared knowledge ensures information captured during patient encounters remains consistent and usable throughout the revenue cycle.
2. Precision and Attention to Detail
Accuracy is essential in both positions. Medical assistants must document patient information correctly. Coding professionals must interpret that documentation precisely. Errors at either stage can result in compliance issues, claim denials, or delays in care coordination.
3. Administrative System Engagement
Both roles spend substantial time working within electronic health record systems and coordinating information across teams. Structured documentation and adherence to workflow processes are critical for maintaining operational continuity.
4. Cross-Functional Collaboration
Medical assistants collaborate with physicians, nurses, and front-office staff. Coding professionals coordinate with revenue cycle teams, payers, auditors, and compliance leaders. Clear communication across these groups supports smoother transitions from care delivery to reimbursement.
5. Organizational Impact
Each role contributes to documentation accuracy, operational efficiency, and regulatory compliance. One strengthens the clinical front end. The other ensures that clinical documentation becomes compliant and reimbursable claims.
The comparison becomes most meaningful when evaluated against performance metrics. Staffing decisions influence outcomes that leadership teams monitor closely, including denial rates and revenue cycle efficiency.
Also Read: Top 10 Medical Billing Companies in the USA
Operational Impact on Revenue Cycle Performance
The difference between medical assistant vs medical billing and coding roles becomes measurable in revenue cycle metrics.
Coding performance directly influences:
- First-pass claim acceptance
- Denial rates
- Days in accounts receivable
- Audit exposure
Medical assistants affect documentation quality at the point of care. Coding professionals determine whether that documentation becomes a clean, compliant claim. When coding capacity does not keep pace with patient volume, denial risk and reimbursement delays increase. Sustainable growth requires aligning staffing strategy with revenue complexity.
When does the data suggest expanding clinical intake support versus strengthening coding capacity? Let’s find out.
When Should You Expand Medical Assistant vs Coding Capacity?
Hiring decisions should follow operational signals.
Expand Medical Assistant Capacity When:
- Patient wait times increase
- Intake documentation lacks completeness
- Provider throughput slows
- Front-office coordination becomes inefficient
Strengthen Coding Capacity When:
- Denial rates trend upward
- First-pass acceptance declines
- A/R days increase
- Coding backlogs delay submission
- Audit findings indicate compliance gaps
Matching staffing decisions to measurable workflow constraints reduces unnecessary expansion and improves performance stability.
Real-World Example: Documentation Volume vs Coding Bottlenecks
A multi-specialty clinic increased patient volume without expanding coding capacity. Documentation volume rose, claim turnaround slowed, and denials increased due to rushed coding and incomplete chart review.
After implementing AI-assisted coding validation, the clinic improved submission speed and reduced denial rates without adding headcount. Scaling patient volume without strengthening coding processes increases risk.
Also Read: Medical Coding Software: Transforming Healthcare Revenue Cycle Management
Staffing adjustments solve part of the problem. Technology addresses the structural gap between documentation and claim submission.
Where AI-Powered Medical Coding Automation Creates Leverage
AI-powered coding platforms strengthen the link between documentation and reimbursement. They improve revenue cycle performance by:
- Validating documentation in real time
- Recommending compliant codes based on payer rules
- Detecting denial patterns before claim submission
- Maintaining structured, audit-ready traceability
- Reducing repetitive manual chart review
Automation does not replace coding expertise. It enhances consistency, improves throughput, and allows organizations to scale without proportional increases in headcount. Effective workforce planning must balance staffing strategy with technology adoption.

Medical Assistant vs Medical Billing and Coding: Compensation and Market Demand
Labor data shows a compensation gap between the two roles. Medical assistants typically earn median salaries in the low-to-mid $44,000 range, while medical records and health information professionals, including coders, earn closer to $53,312 annually.
The difference reflects the regulatory accountability and financial impact tied to coding accuracy.
Demand for medical assistants continues to rise with outpatient growth. Coding roles remain critical as reimbursement requirements become more complex and payer oversight intensifies.
Career Mobility
Medical assistants may advance by specializing in clinical areas or pursuing further education in nursing or other licensed roles.
Medical billing and coding professionals often progress into:
- Coding audit and quality assurance positions
- Compliance and regulatory oversight roles
- Revenue cycle leadership
Advancement in coding typically requires additional certifications and demonstrated expertise in complex documentation and payer guidelines.
As coding responsibilities grow more complex, the operational strain on revenue cycle teams increases. Expanding staff alone may not keep pace with rising documentation volume and evolving CMS requirements.
This is where technology becomes part of the long-term strategy. Platforms like RapidClaims support coding teams with AI-driven automation designed to improve accuracy, reduce denials, and maintain audit readiness.
RapidClaims: AI-Powered Medical Coding Automation
RapidClaims is an enterprise AI platform built to improve coding accuracy, reduce denials, and strengthen compliance across healthcare organizations. It supports revenue cycle teams by combining automation with structured validation.
Key Features
- AI-Assisted Code Assignment: Analyzes clinical documentation and suggests compliant ICD-10, CPT, and HCPCS codes.
- Real-Time Documentation Validation: Identifies gaps and inconsistencies before claim submission.
- Denial Risk Detection: Flags patterns linked to rejections to improve first-pass acceptance.
- Audit-Ready Reporting: Maintains traceable coding logic to support compliance reviews.
- EHR Integration: Integrates into existing workflows without disrupting operations.
By combining experienced coding professionals with intelligent automation, healthcare organizations can scale revenue performance while maintaining accuracy and compliance.

Conclusion
The comparison between medical assistant vs medical billing and coding ultimately comes down to workflow ownership and revenue accountability.
Medical assistants ensure documentation is captured accurately at the point of care. Coding professionals translate that documentation into compliant, reimbursable claims. When the handoff between these roles breaks down, denial rates rise, and reimbursement timelines extend.
As regulatory requirements grow more complex, manual processes alone cannot support sustainable scale. AI-powered medical coding automation strengthens accuracy, reduces rework, and maintains audit readiness without continuous headcount expansion.
Learn how RapidClaims supports high-accuracy, compliant claim submission for modern healthcare organizations. Request a demo now!
FAQs
1. What is the difference between a medical biller and a medical assistant?
A medical assistant supports clinical care and front-office operations. A medical biller focuses on claims submission, payment tracking, and reimbursement workflows within the revenue cycle.
2. What’s the difference between MA and MAA?
MA typically refers to a Medical Assistant. MAA often stands for Medical Administrative Assistant, a role focused more on scheduling, records, and front-desk operations rather than clinical tasks.
3. What is better, CMA or CCMA?
CMA (Certified Medical Assistant) and CCMA (Certified Clinical Medical Assistant) are both recognized credentials. The better option depends on employer preference and whether the role emphasizes broader administrative duties or clinical focus.
4. What is the highest level of medical assistant?
There is no universal “highest” level, but senior or lead medical assistants may supervise teams. Advancement often requires additional certifications or transition into nursing or healthcare management roles.
5. Which role has a bigger impact on claim denials?
Coding professionals directly influence claim accuracy and denial rates. Medical assistants impact denials indirectly through the completeness and clarity of documentation.
6. Can medical assistants perform medical coding?
They may assist with documentation tasks, but assigning diagnosis and procedure codes requires formal education and certification aligned with regulatory standards.
7. Which role has a greater impact on revenue cycle performance?
Medical billing and coding professionals have a direct impact on reimbursement timelines, denial rates, and financial performance.
.png)
Mary Degapogu
Mary Degapogu is a proficient medical coder with 6 years of experience in E/M Outpatient and ED Profee coding, focused on precise code assignment and documentation compliance to drive clean claims and revenue integrity at RapidClaims.
Latest Post
expert insights with our carefully curated weekly updates
Related Post
Top Products

%201.png)