What is E/M Coding? A Complete Guide to E/M Services
.jpg)
Is Inaccurate Coding Causing Revenue Loss and Compliance Issues in Your Healthcare Practice?
Evaluation and Management (E/M) coding plays a crucial role in addressing these challenges. Accurate E/M coding ensures proper reimbursement and helps maintain compliance. The 2024 Medicaid improper payment estimate dropped to 5.09%, reflecting a decline due to improved coding practices, as noted by the Georgetown University Center for CCF. This highlights the importance of precise E/M coding in ensuring financial stability and regulatory compliance.
In this blog, you’ll learn how refining your E/M coding processes can help overcome these challenges and keep your practice financially stable and compliant.
TL;DR (Key Takeaways)
- E/M coding (99202–99499) standardizes billing for evaluation and management services using MDM, time, history, and exam.
- Codes are grouped by service type: office, hospital, emergency, critical care, nursing facility, preventive, prolonged, and neonatal.
- Exclusions include diagnostic tests, procedures, preventive services, and bundled surgical care, which require separate reporting.
- Patient status (new vs. established) and provider type (QHP vs. clinical staff) directly affect code selection and reimbursement accuracy.
- Unlisted services (99429, 99499) require detailed special reports to justify necessity and secure reimbursement.
What is E/M Coding?
Evaluation and Management (E/M) coding plays a critical role in healthcare billing, ensuring that physicians and other healthcare professionals are reimbursed for their services. E/M codes, ranging from 99202 to 99499, are used to represent services focused on evaluating and managing a patient’s health.
E/M services cover a broad range of healthcare activities, and accurate coding is crucial for reimbursement. These codes are accepted by Medicare, Medicaid, and private insurers, making them essential for financial operations in healthcare settings.
Major updates were introduced in 2021 for office/outpatient E/M coding rules, with further changes in CPT E/M Code and Guideline Changes effective January 1, 2023, by the American Medical Association (AMA).
Understanding the Structure of a Typical E/M Code
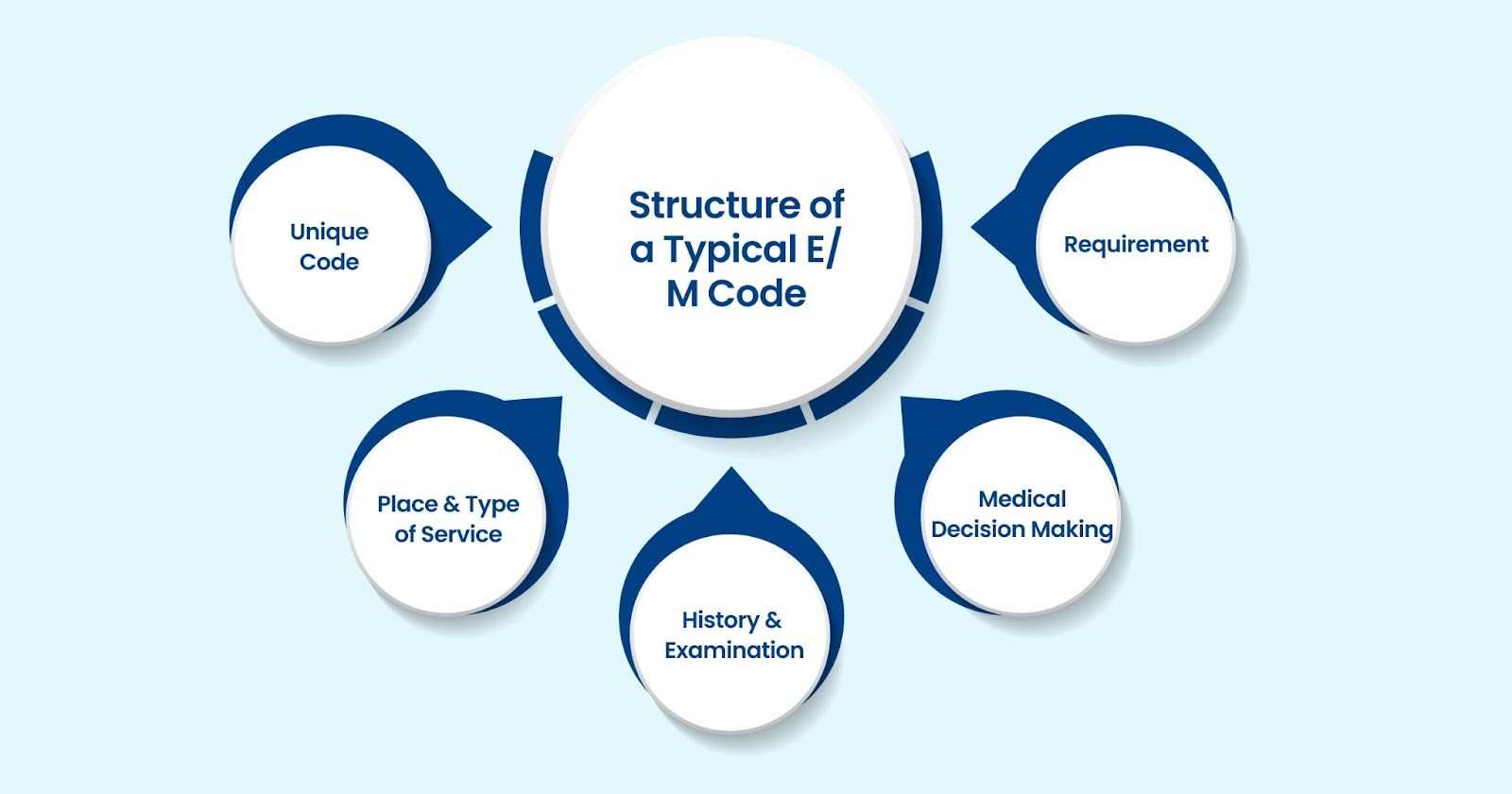
CPT is a set of five-character medical codes maintained by the AMA, covering various medical specialties, including E/M. Other sections in the CPT codes set include Anesthesia, Surgery, Radiology, Pathology, and Medicine. E/M codes represent services provided during patient encounters. These codes follow a standardized format, with the level of service determined by specific factors.
Here's an overview of what a typical E/M code includes:
- Unique Code: Each E/M code has a specific number, like 99235.
- Place and Type of Service: This refers to where the service is provided (e.g., hospital inpatient or outpatient) and the nature of the service (e.g., observation care, same-day admission and discharge).
- History and Examination: The code requires a medically appropriate history and/or physical examination based on the patient’s condition.
- Medical Decision Making (MDM): The level of decision-making required, which could be categorized as low, moderate, or high. For example, a moderate level of MDM is often required.
- Requirement: Some codes are based on the total time spent with the patient. For instance, a code may require a minimum of 70 minutes to be met on the date of the encounter.
Example of an E/M Code: For instance, the code 99235 could be used for hospital inpatient or observation care, where the evaluation and management of the patient includes both admission and discharge on the same date. This code requires:
- A medically appropriate history and/or examination
- A moderate level of medical decision-making (MDM)
- A minimum of 70 minutes of total time spent with the patient on the date of the encounter.
This is the typical format for many commonly used E/M codes.
Updates to E/M Codes
- 2021 Revisions: Significant changes were made to office and outpatient E/M codes 99202-99215 to simplify documentation requirements and align coding with the level of medical decision making (MDM) or total time, rather than focusing on history and examination alone.
- 2024 Revisions: These updates further clarified the time requirements, shifting from a time range to a minimum time that must be met or exceeded for code selection. However, 99211, for established patients, does not require a time-based selection.
Understanding the structure and updates to these E/M codes is essential for accurate coding and ensuring proper reimbursement for healthcare services.
Detailed Overview of E/M Code Categories
The CPT code range for Evaluation and Management (E/M) services spans 99091 to 99499, covering various types of patient encounters. Below is an overview of the key E/M code categories:
Important Terminology in E/M Coding

Understanding the essential terms used in E/M coding is crucial for accurate billing and compliance. Here are some definitions to help you better understand the terminology used in E/M coding:
1. Qualified Healthcare Professional (QHP)
A QHP is an individual who has the necessary education, training, licensure, and facility privileges (if applicable) to perform professional services within their scope of practice. According to CPT guidelines, they can report their professional services independently. This includes roles like advanced practice nurses (APNs) and physician assistants (PAs).
2. Clinical Staff Member
A clinical staff member is someone who works under the supervision of a QHP and can perform or assist in performing specific professional services, as permitted by law, regulation, and facility policy. However, unlike QHPs, clinical staff members cannot report these services independently.
3. Professional Service
In the context of E/M coding, a professional service is defined as a face-to-face service provided by a QHP, who is responsible for reporting the corresponding E/M codes. This term helps distinguish between new and established patients when assigning E/M codes.
4. New Patient
A new patient is someone who has not received professional services from the physician or healthcare professional providing the current service in the past three years. If the patient has not received services from another professional of the same specialty or subspecialty within the same practice, they are also considered new.
For Medicare, only the same specialty (not subspecialty) is considered when determining if a patient is new for E/M purposes.
Example: If a 65-year-old male visits a cardiologist for a new E/M service, and although another cardiologist from the same practice interpreted an EKG for the same patient the previous year during an emergency visit (without face-to-face contact), the patient is still considered "new" for E/M purposes since the same cardiologist provided no direct, face-to-face service.
5. Established Patient
An established patient has received professional services from the physician or healthcare provider within the past three years, or from another healthcare provider within the same specialty and subspecialty, if applicable, within the same group practice.
Example: If a pediatric patient visits a pediatric gastroenterologist complaining of stomach pain, but another gastroenterologist in the same practice saw the patient two years ago for a similar complaint, the patient is considered established for this visit.
Accurate documentation of these elements ensures the correct E/M code is used, optimizing reimbursement and compliance. RapidClaims, an AI-driven coding automation platform, simplifies this by using the latest guidelines and MDM analysis. Its MDM solver accurately determines the complexity of medical decision-making, helping providers select the appropriate E/M levels and streamline the coding process.
Understanding the Levels of E/M Services
Each E/M code category or subcategory typically contains three to five levels, each with its own specific code. These levels are designed to capture variations in the skills, knowledge, work, and time required for different types of encounters.
For most E/M services, the Medical Decision Making (MDM) level or the total time spent with the patient determines the appropriate code level. Here are key points to consider when selecting the right E/M code:
- MDM or Time Determines Code Level: The level of MDM or the time spent with the patient often dictates the code to use. Higher complexity in decision-making or more time spent with the patient typically corresponds to a higher-level code.
- Time Not Applicable for All Services: For some services, such as Emergency Department (ED) visits, time isn't used to determine the code. ED services are typically high-volume, and time for individual patients can be difficult to calculate.
- Different Component Requirements for Same-Level Codes: Even if two E/M codes are at the same level, the specific requirements for each code may differ. Always review the code descriptions carefully to ensure the correct selection.
The table below illustrates how E/M component requirements can differ even between two codes within the same level. Both codes require a medically appropriate history, examination, and a straightforward or low level of MDM, but the time requirement varies. For example, 99221 requires at least 40 minutes, while 99231 requires 30 minutes.
Accurately selecting the appropriate E/M code ensures proper reimbursement and compliance. Understanding the differences in time, MDM, and requirements helps streamline the coding process for your practice.
Accurately selecting the appropriate E/M code ensures proper reimbursement and compliance. To streamline this process, healthcare providers can benefit from advanced tools like RapidClaims. This AI-driven coding automation platform enhances accuracy, ensures compliance, and minimizes errors. With features like intelligent MDM analysis, time-based coding, and a customizable workflow, RapidClaims helps reduce claim rejections and optimize reimbursement.
What Is Excluded from E/M Codes?

Understanding what E/M codes do not include is as important as knowing the factors that affect E/M code selection. Here are key points to keep in mind:
1. Diagnostic Tests and Studies
You may report the performance and interpretation of diagnostic tests and studies separately, as long as the documentation meets the requirements for separate reporting under the corresponding codes.
2. Procedure and Service Codes
You may report a procedure or service code alongside an E/M code for a significant, separately identifiable service. However, the work done for the procedure or service should not be counted in determining the E/M code level. If reporting an E/M code with a procedure, apply modifier 25 to indicate that the E/M service was separate and significant.
3. Preventive Services
Preventive care services, such as routine physical exams or immunizations, are not considered part of E/M services unless additional issues or concerns are addressed during the visit that require separate E/M reporting.
4. Global Surgical Packages
E/M services related to a global surgical package, like pre-operative visits or follow-up care during the global period, are generally bundled into the procedure code and should not be reported separately.
By understanding these exclusions, coders can ensure accurate billing and avoid reporting errors that can impact reimbursement and compliance. Platform like RapidClaims simplifies E/M coding with AI-powered automation, determining reimbursement levels based on visit complexity. With continuous updates in coding standards (ICD-10, CPT, HCPCS, HCC, E&M), RapidClaims keeps your coding accurate and up-to-date, streamlining the entire process.
Also Read: Intro to Commonly Used Medical CPT/HCPCS Codes List.
Unlisted E/M Services and the Importance of Special Reports
Some services may not have a specific code in the CPT code set, and these should be reported using 99429 for unlisted preventive medicine services or 99499 for unlisted E/M services. When reporting these services, a special report is required to describe the service in detail.
A special report is essential documentation that justifies the medical necessity of an unlisted or unusual service. This report should include:
- The nature, extent, and need for the service.
- The time, effort, and equipment required for the service.
- Additional details include complex symptoms, the final diagnosis, relevant physical findings, procedures performed, concurrent problems, and follow-up care.
When submitting special reports to payers, it is highly recommended to use plain language to ensure the information is understandable, even for non-experts. This helps avoid confusion and provides a smoother review process.
RapidClaims, an AI-driven medical coding automation platform, enhances the accuracy and efficiency of E/M coding through its autonomous coding system, complemented by AI-assisted recommendations. The platform streamlines the claim submission process, ensuring timely and precise coding, and seamlessly integrates into existing systems to optimize the revenue cycle.
Conclusion
Understanding what is E/M coding is essential for accurate billing and reimbursement in healthcare. By mastering the components, guidelines, and code selection, providers can ensure compliance and optimize revenue. Accurate E/M coding helps maintain financial stability and regulatory adherence in medical practices.
RapidClaims takes this a step further. With features like real-time code validation, seamless EHR integration, and predictive search, the platform provides a reliable and intuitive way to simplify complex billing workflows. Additional tools such as RapidCode, RapidAssist, and RapidRisk further strengthen this system by automating documentation, improving coding precision, reducing claim denials, and supporting a healthier revenue cycle.
As coding guidelines for CPT codes and insurance requirements continue to evolve, using an intelligent tool like RapidClaims ensures your code selections remain accurate, compliant, and up to date.
Looking to improve the accuracy and efficiency of your E/M coding? Let RapidClaims streamline your medical coding process and optimize your billing operations. Request a Free Demo to See the Tool in Action.
Frequently Asked Questions (FAQs)
1. Can I report diagnostic tests separately from an E/M service, and under what conditions?
Yes, diagnostic tests and studies can be reported separately from an E/M service, as long as the documentation meets the requirements for separate reporting under the corresponding codes.
2. How should I report a procedure code along with an E/M service on the same day?
You can report a procedure code alongside an E/M code if the service is significant and separately identifiable. To indicate this, use modifier 25 to show that the E/M service was separate and significant from the procedure.
3. Are preventive services, such as routine exams or immunizations, included in E/M coding?
Preventive services like routine physical exams or immunizations are generally not part of E/M services unless additional issues or concerns are addressed during the visit that require separate E/M reporting.
4. Can I report a telemedicine visit with the same E/M codes used for in-person visits?
Yes, telemedicine visits can be reported using the same E/M codes as in-person visits, provided that the documentation meets the same requirements and the service is medically necessary.
5. What happens if I use the wrong E/M code level?
Using the wrong E/M code level can lead to underbilling (resulting in lost revenue) or overbilling (leading to audits, penalties, or compliance issues). It’s essential to ensure that the code matches the complexity of the service provided.
6. Do I need to update E/M codes for follow-up visits with a patient?
Yes, follow-up visits are typically assigned a level based on the ongoing complexity of the patient’s condition, treatment progress, and the decision-making required during the visit. Documentation should reflect any changes or updates in the patient's condition.

Muyied Ulla Baig
Muyied Ulla Baig is a dedicated medical coder with 1 year of experience in E/M Outpatient, HCC, and Dental coding, supporting accurate risk adjustment and claims integrity through detailed and compliant coding processes at RapidClaims.
Latest Post
expert insights with our carefully curated weekly updates
Related Post
Top Products

%201.png)

.jpg)
.jpg)





