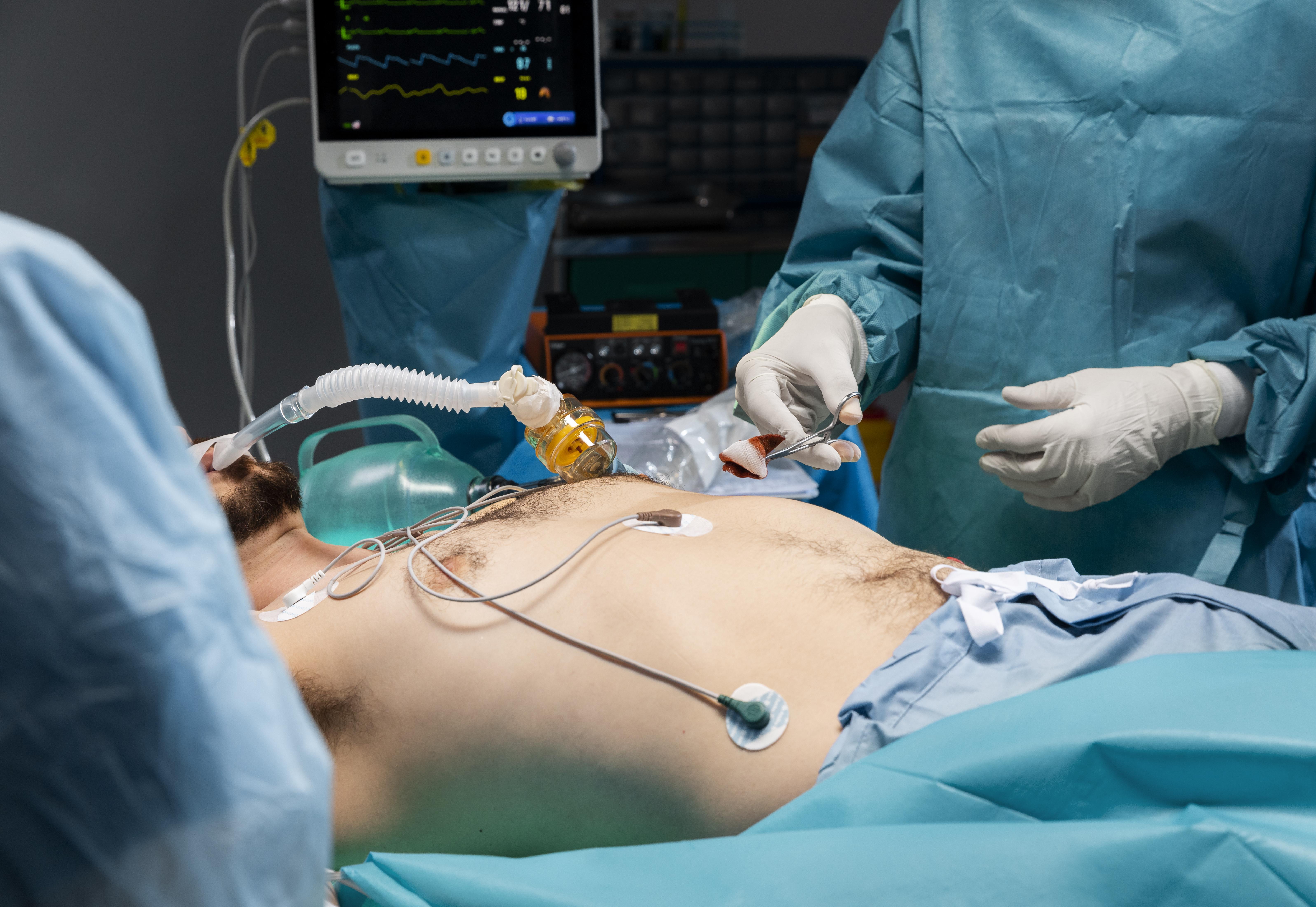
When 26 Claims Cost $12.1 Million: OIG Audit Reveals What Healthcare Leaders Cannot Afford to Ignore
The February 2026 OIG audit of Sarasota Memorial Hospital is one of the most instructive compliance cases in recent memory. Not because of the dollar figure. Because of what caused it.
Sarasota Memorial is not a hospital that neglected compliance. Five-star CMS quality rating. Leapfrog A grades year after year. Utilization review nurses, physician advisors, real-time dashboards, quarterly PEPPER reviews. The infrastructure was there. The policies were written. The training was happening. By every visible measure, this was an organization that took compliance seriously.
And still, a federal audit found a multi-million dollar overpayment exposure across two years of claims.
The root cause OIG identified was not fraud. It was not a missing program. Staff did not consistently follow the hospital's own written policies and procedures. That sentence is worth sitting with. Because what it is really saying is that the distance between a policy that exists and one that executes consistently at scale, across thousands of claims, under daily operational pressure, is wider than most organizations want to admit.
The errors were not random either. They concentrated in specific, well-known risk areas. Short-stay inpatient admissions where the physician's clinical rationale at the time of the order was not sufficiently captured in the documentation. Inpatient rehabilitation admissions where the complexity justifying that level of care was not established clearly enough at the point of admission. Outpatient claims where billing modifiers were applied without the clinical documentation to support them. These are not new risk categories. They appear in OIG work plans every year. The standards are published and widely known. This was not a knowledge problem. It was an execution problem.
And execution problems do not show up in your denial rate.
This is the part most revenue cycle teams underweight, and it is simpler than the compliance mechanics. The claims at the center of this audit were paid. They cleared payer editing. They generated no denials. From a standard revenue cycle reporting perspective, they looked completely clean. The liability only became visible when an independent medical reviewer applied federal billing criteria to the supporting documentation years after the service date. Most organizations have robust infrastructure for tracking what payers reject. Far fewer have meaningful visibility into what federal auditors might recover from claims that were already paid. Those are not the same problem. They are not caught by the same controls. Denial rate performance and OIG audit exposure can coexist comfortably while the gap quietly compounds. A clean denial rate does not mean clean claims. It means payers did not flag them. That is a different standard than the one applied in a post-payment federal audit.
When the hospital pushed back during the appeals process with additional clinical documentation, OIG revised its findings downward. The documentation that changed the outcome already existed. It just was not visible in the original record. Which means better upstream documentation discipline would have been more protective than the appeals process that partially recovered it. The gap was not clinical. It was documentation.
The time dimension adds another layer most organizations are not modeling. Admission decisions from 2020 were adjudicated in 2026. That is not exceptional. That is how post-payment review works. The compliance infrastructure in place today is not only protecting current claims. It is building the evidentiary record for decisions that may be examined years from now under scrutiny that cannot be fully anticipated.
The takeaway from Sarasota Memorial is not that compliance programs do not work. It is that they are necessary and insufficient. What sits between a program that functions and one that holds under federal audit scrutiny is consistent execution at the claim level, in every service line, on every high-risk claim category, documented at the moment of the clinical decision. That is harder to build than a policy. It is harder to measure than a denial rate. And it is exactly where the risk lives.
RapidClaims helps health systems and physician groups maintain coding accuracy and audit defensibility across the full claims lifecycle. If the Sarasota Memorial findings raise questions about your organization's exposure, we are glad to talk through what continuous coding oversight looks like in practice.

Team RapidClaims
Latest Post
expert insights with our carefully curated weekly updates
Related Post
Top Products

%201.png)