

Recover more from every
denied and underpaid claim
Stop leaving denied and underpaid revenue on the table.
RapidRecovery works every claim, end to end
Introducing RapidRecovery
Purpose-built for healthcare revenue cycle teams to recover
revenue owed to them
The real cost of denials
70%
Of claims are either denied
or delayed
$25.7B
Spent annually on claims adjudication
up by 30%
Increase in admin cost per denied claim
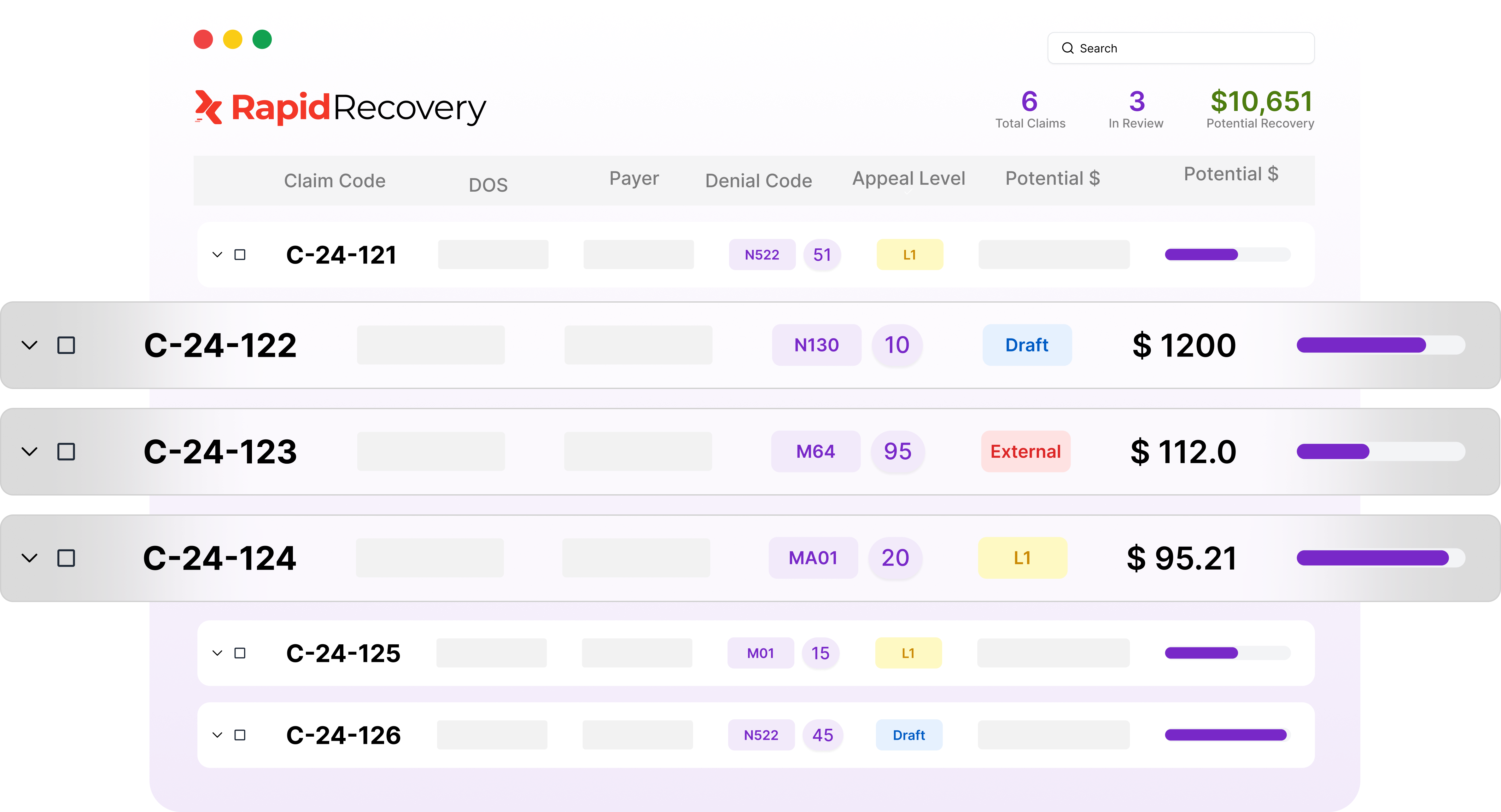
Stop Denials Before
They Start
Every denial worked by RapidRecovery feeds back into your pre-claim workflow as an edit within 24 hours. The more claims it processes, the fewer denials reach a payer.
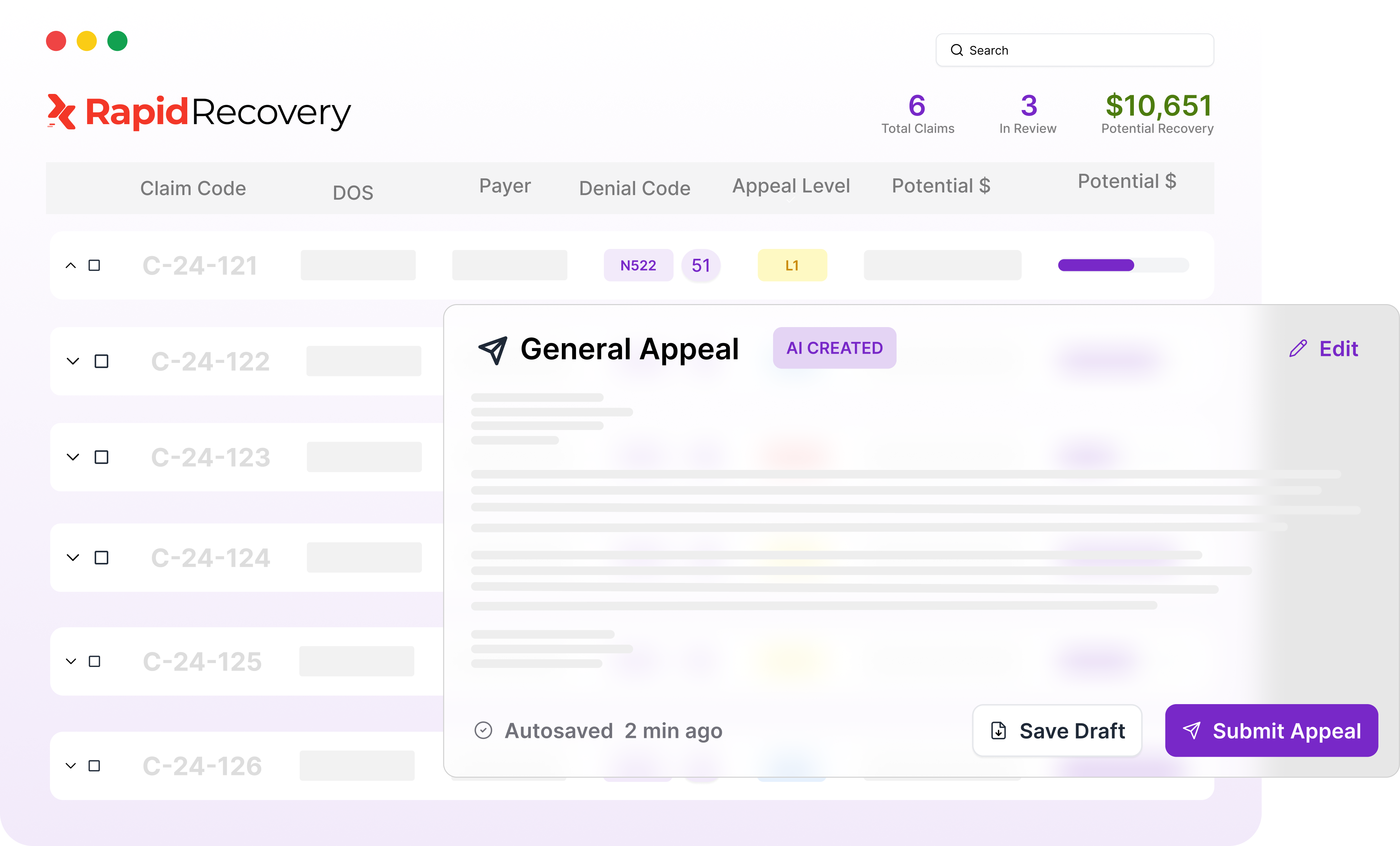
Make Every Appeal Count
AI drafts payer-specific appeal letters, built around each payer's rules, documentation requirements, and claim history, so every appeal is complete, accurate, and defendable.
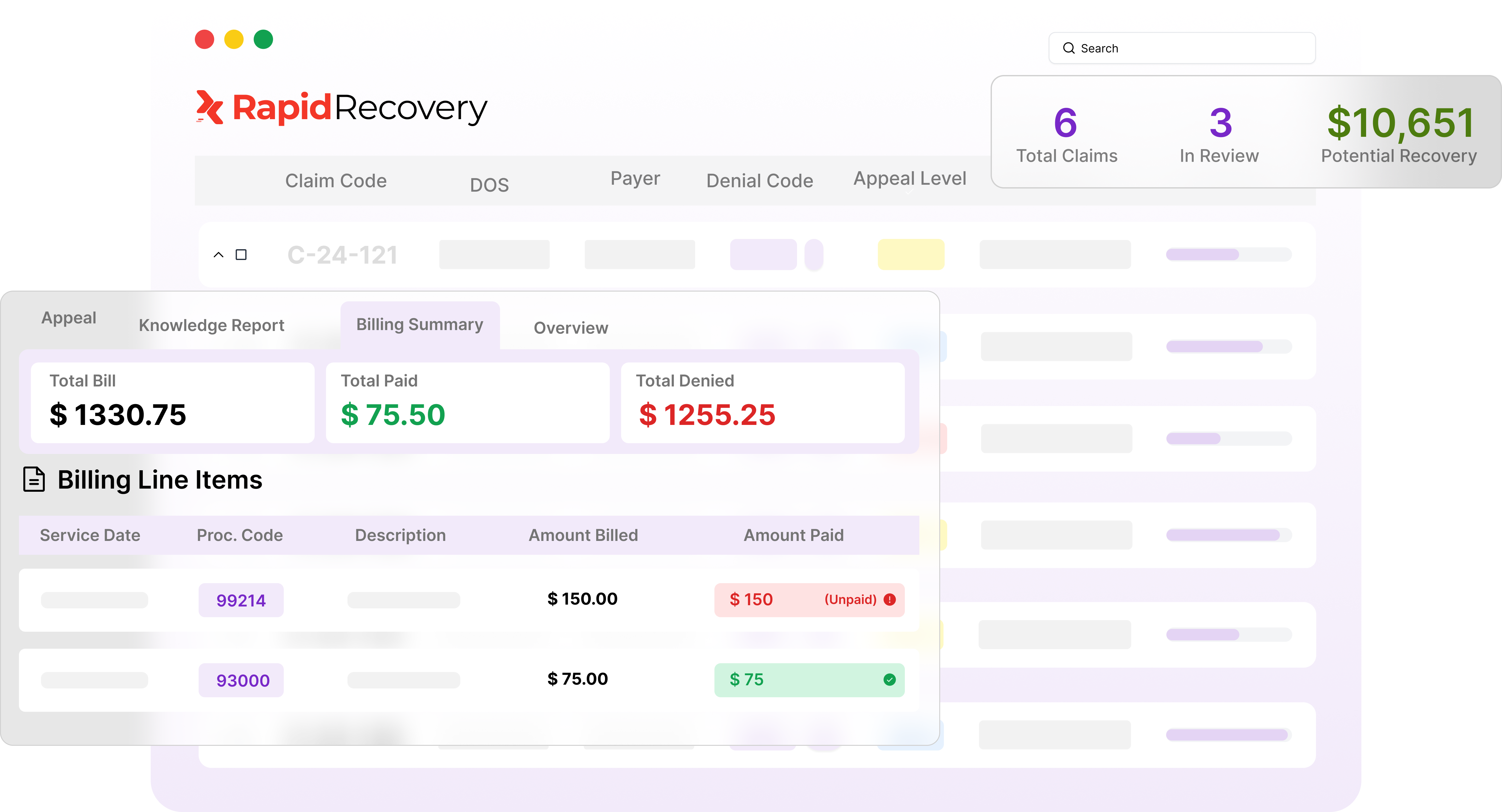
Close the Gap Between Denied and Paid
Our AI agents call payers directly, uncovers denial reasons, and handles live objections, autonomously or alongside your team. Cash moves faster without your team chasing every claim.
Your Workflow, On Autopilot
ML risk scoring routes every claim intelligently, sending high-risk claims to human reviewers and clearing low-risk ones straight to the payer. Dynamic worklists give your team clarity on what needs attention and the automation to act on it.
Results we’ve delivered
68%Overturn Rate under 30 days
Large Health System with
1.3M Denials / year
55%appeal success rate$1.05M recouped
Multispecialty Group - 250k denials / year
6.4X ROIWithin 90 days
Community Hospital Network
Plug In.Not Start Over.
RapidRecovery integrates to your existing EHR and billing systems so you see results without
disrupting how your team works.


Get your denials recovered today
See how RapidRecovery creates predictability and revenue growth
Purpose-Built for Your Organization
Contact us to see how we can work with your organization.
contact us
Our Platform Integrates with All Major EHR Systems
Request a Demo
%201.png)






















Transform Your Revenue Cycle in 30 Days or Less
Join leading healthcare organizations already seeing results with RapidClaims.






