Healthcare CFOs Are Being Asked to Predict an Unpredictable Industry
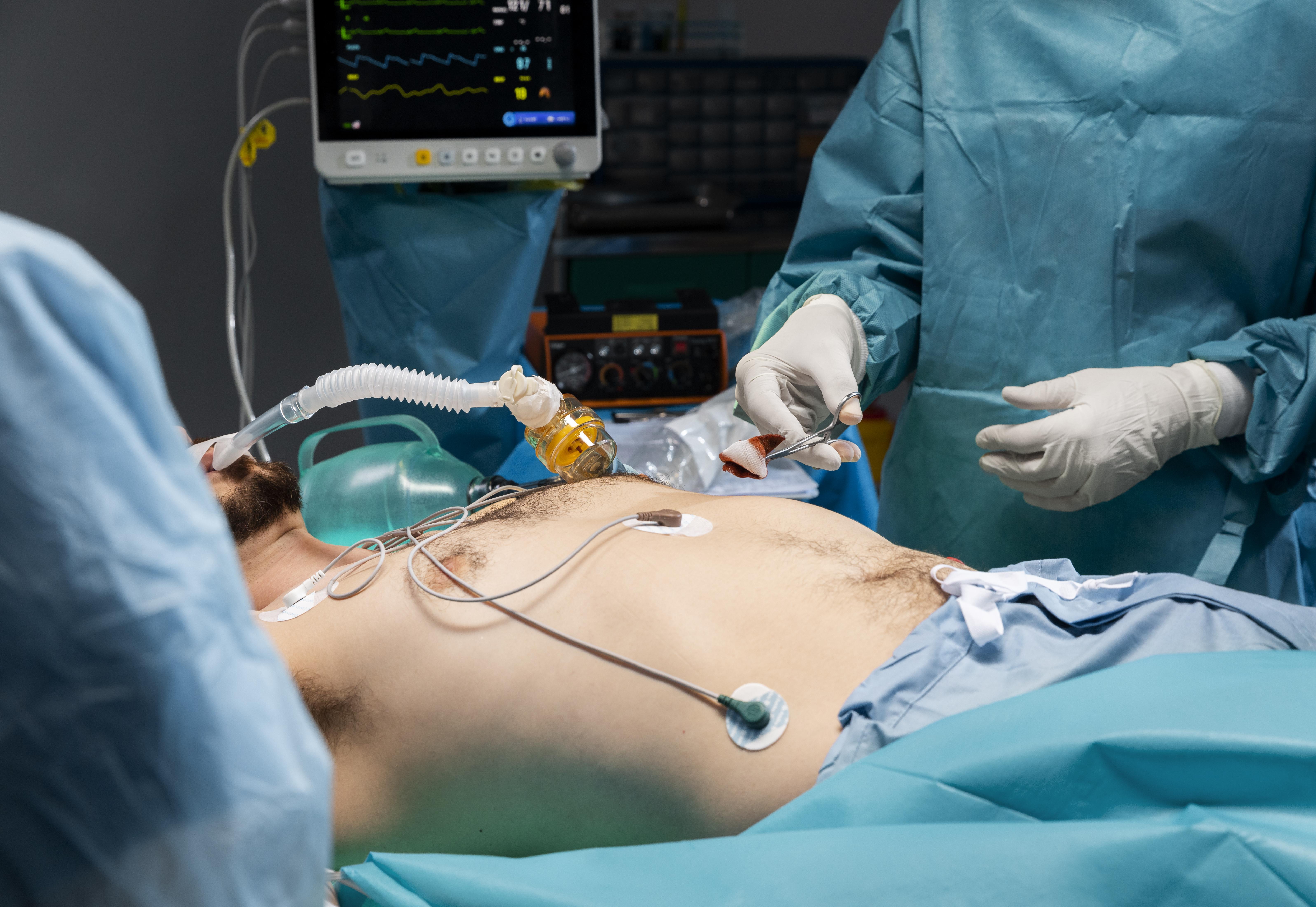
At 7:12 a.m., the hospital CFO is already behind.
Overnight census numbers are up. Good news clinically, complicated news financially. Higher volume improves revenue projections, but staffing costs will follow. A quick glance at the dashboard shows A/R holding steady, but one payer's remittance file is late again. That alone won't break the month. Unless it becomes a pattern. Patterns are what keep finance leaders cautious.
By 9 a.m., the forecast meeting begins. The spreadsheet assumes stability. Historical yield, expected case mix, normal payment cadence. The math is clean. The assumptions are not.
A single policy change from a major payer can quietly distort an entire quarter. A documentation clarification can shift reimbursement timing without touching volume. A denial trend can appear small at first and compound across thousands of encounters before anyone calls it systemic. None of this shows up in the forecast model until it's already happening.
Healthcare asks finance leaders to produce precise predictions inside a system that behaves probabilistically. That tension defines the modern CFO role.
In most industries, forecasting is an exercise in trend analysis. Demand fluctuates, but payment structures are stable. Receivables convert within predictable ranges. Variance exists, but it's bounded.
Healthcare finance operates in a moving environment. Payment depends not only on activity but interpretation. Rules evolve midstream. Automation increases scrutiny. Regulatory pressure shifts documentation standards. Clinical reality moves faster than reimbursement logic can follow.
The pressure intensifies under private equity ownership. Investors expect operational discipline and financial predictability. Debt structures assume cash conversion behaves within modeled ranges. Variance is no longer just an internal planning issue. It becomes a capital markets signal.
A forecast miss in this environment is not treated as noise. It's treated as governance.
The CFO becomes the translator between an inherently unstable payment ecosystem and stakeholders who require steady financial narratives. That requires more than technical accuracy. It requires judgment about uncertainty itself.
The strongest healthcare finance teams are not the ones that eliminate volatility. That's impossible. They're the ones that understand its shape. They plan for variance instead of assuming it away. They treat reimbursement behavior as a variable to be monitored continuously, not a backdrop to be accepted passively.
This means shifting from prediction to detection. Instead of asking "What will our denial rate be next quarter?" The better question is "How fast will we know if our denial rate is trending wrong, and what can we do about it?"
Real-time visibility into revenue cycle performance becomes essential. Not monthly reports that show what happened six weeks ago, but daily indicators that flag problems while there's still time to intervene. Pattern recognition across payers that alerts finance teams when one payer starts denying claims at a higher rate immediately, not after it impacts the quarterly close.
The job is no longer just about precision. It's about resilience under scrutiny.
Because in an industry where the rules can shift quietly and the cash follows slowly, the real measure of financial leadership is not predicting the future perfectly. It's staying credible when the future refuses to cooperate.
That credibility comes from building revenue cycle operations around agility - real-time data, proactive monitoring, rapid response protocols. Organizations that continue treating revenue cycle as a static planning exercise will continue missing targets and scrambling to explain why.
The industry isn't getting more predictable. The question is whether your finance team has the infrastructure to navigate uncertainty without losing credibility.
Ready to Build Revenue Cycle Resilience?
Let's talk about building resilience into your revenue cycle.

Team RapidClaims
Latest Post
expert insights with our carefully curated weekly updates
Related Post
Top Products

%201.png)